Abstract
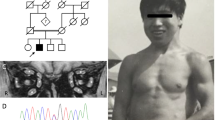
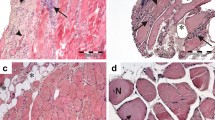
To clarify the muscle pathology findings of a 39-year-old female Chédiak-Higashi syndrome (CHS) case with diffuse limb muscle atrophy, histochemical and electron microscopic studies were performed. In addition to neurogenic muscle atrophy due to the peripheral neuropathy, the most striking change seen by light microscopy was the widespread appearance of acid phosphatase-positive granules in many normal-looking muscle fibers. Coincident with the histocemical findings, electron microscopy showed many autophagic vacuoles containing glycogen particles and membranous structures in almost all muscle fibers. Although further studies are necessary, diffuse distribution of acid phosphatase-positive granules (autophagic vacuoles) in the skeletal muscle may reflect one of the generalized lysosomal abnormalities in CHS.
Similar content being viewed by others
References
Banker BQ (1986) The pathology of the motor neuron disorders. In: Engel AG, Banker BQ (eds) Myology, vol 2. McGraw-Hill Book Company, New York, pp 2031–2067
Béguez-Cesar BA (1943) Neutropénia cronica maligna familiare con granulaciones atipicas de los leucocitos. Bol Soc Cuban Pediatr 15:900–922
Blume RS, Wolff SM (1972) The Chédiak-Higashi syndrome: studies in four patients and a review of the literature. Medicine 51:247–280
Chédiak M (1952) Nouvelle anomalie leucocytaire de caractere consistitutionnel et familial. Rev Hematol 7:362–367
Dent PB, Fish LA, White JG, Good RA (1966) Chédiak-Higashi syndrome. Observation on the nature of the associated malignancy. Lab Invest 15:1634–1642
DiMauro S, Hartlage PL (1978) Fatal infantile form of muscle phosphorylase deficiency. Neurology 28:1124–1129
DiMauro S, Hartwig GB, Hays A, Eastwood AB, Franco R, Olarte M, Chang M, Roses AD, Fetell M, Schoenfeldt RS, Stern LZ (1979) Debrancher deficiency: neuromuscular disorder in 5 adults. Ann Neurol 5:422–436
Donohue WL, Bain HW (1957) Chédiak-Higashi syndrome. A lethal familial disease with anomalous inclusions in the leukocytes and constitutional stigmata: report of a case with necropsy. Pediatrics 20:416–430
Haliotis T, Roder J, Klein M, Ortaldo J, Fauci AS, Herberman RB (1980) Chédiak-Higashi gene in humans. I. Impairment of natural-killer function. J Exp Med 151:1039–1048
Hays AP, Hallett M, Delfs J, Morris J, Sotrel A, Shevchuk MM, DiMauro S (1981) Muscle phosphofructokinase deficiency: abnormal polysaccharide in a case of late-onset myopathy. Neurology 31:1077–1086
Higashi O (1954) Congenital gigantism of peroxidase granules. The first case ever reported of qualitative abnormality of peroxidase. Tohoku J Exp Med 59:315–332
Ito J, Tokumaru M, Okazaki T (1972) Chédiak-Higashi syndrome: report of a case with autopsy and electron microscopic studies. Acta Pathol Jpn 22:755–777
Karpati G, Carpenter S, Eisen A, Aubé Michel DiMauro S (1977) The adult form of acid maltase (α-1,4-glucosidase) deficiency. Ann Neurol 1:276–280
Klein M, Roder J, Haliotis T, Korec S, Jett JR, Herberman RB, Katz P, Fauci AS (1980) Chédiak-Higashi gene in humans. II. The selectivity of the defect in natural-killer and antibodydependent cell-mediated cytotoxicity function. J Exp Med 151:1049–1058
Kritzler RA, Trener JY, Lindenbaum J, Magidson J, Williams R, Preisig R, Philips GB (1964) Chédiak-Higashi syndrome-Cytologic and serum lipid observations in a case and family. Am J Med 36:583–594
Kumamoto T, Fukuhara N, Nagashima M, Kanda T, Wakabayashi M (1982) Distal myopathy. Histochemical and ultrastructural studies. Arch Neurol 39:367–371
Larsen WG (1967) The Chédiak-Higashi syndrome and aleutian mink. Arch Dermatol 96:330–331
Lockman LA, Kennedy WR, White JG (1967) The Chédiak-Higashi syndrome: electrophysiological and electron microscopic observation on the peripheral neuropathy. J Pediatr 70:942–951
Maeda K, Sueishi K, Iida M (1989) A case report of Chédiak-Higashi syndrome complicated with systemic amyloidosis and olivo-cerebellar degeneration. Pathol Res Pract 185:231–237
Mastaglia FL, Papadimitriou JM, Dawkins RL, Beveridge B (1977) Vacuolar myopathy associated with chloroquine, lupus erythematosus and thymoma. J Neurol Sci 34: 315–328
Matsuishi T, Yoshino M, Terasawa K, Nonaka I (1984) Childhood acid maltase deficiency: a clinical, biochemical, and morphologic study of three patients. Arch Neurol 41:47–52
Nonaka I, Sunohara N, Ishiura S, Satoyoshi E (1981) Familial distal myopathy with rimmed vacuole and lamellar (myeloid) body formation. J Neurol Sci 51:141–155
Page AR, Berendes H, Warner J, Good RA (1962) The Chédiak-Higashi syndrome. Blood 20:330–343
Roder JC, Haliotis T, Klein M, Korec S, Jett JR, Ortaldo J, Heberman, Katz P, Fauci AS (1980) A new immunodeficiency disorder in humans involving NK cells. Nature 284:553–555
Sato A (1955) Chédiak-Higashi's disease. Probable identity of “a new leucocytal anomaly” (Chédiak) and “congenital gigantism of peroxidase granules” (Higashi). Tohoku J Exp Med 61:201–210
Steinbrinck W (1948) Über eine neue Granulationsanomalie der Leukocyten. Dtsch Arch Klin Med 193:577–581
Sung JH, Meyers JP, Stadlan EM, Cowen D, Wolf A (1969) A neuropathological change in Chédiak-Higashi disease. J Neuropathol Exp Neurol 28:86–118
Tobin WE, Huijing F, Porro RS, Salzman RT (1973) Muscle phosphofructokinase deficiency. Arch Neurol 28:128–130
Trend PSJ, Wiles CM, Spencer GT, Morgan-Hughes JA, Lake BD, Patrick AD (1985) Acid maltase deficiency in adults. Diagnosis and management in five cases. Brain 108:845–860
Witkop CJ Jr, Quevedo WC Jr, Fitzpatrick TB, King RA (1989) Albinism. In: Scriver CR, Beaudet AL, Sly WS, Valle D, (eds) The metabolic basis of inherited disease, 6th edn. McGraw-Hill, New York, pp 2905–2947
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Uchino, M., Uyama, E., Hirano, T. et al. A histochemical and electron microscopic study of skeletal muscle in an adult case of Chédiak-Higashi syndrome. Acta Neuropathol 86, 521–524 (1993). https://doi.org/10.1007/BF00228590
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00228590