Abstract
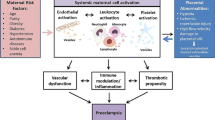
Preeclampsia (PE) is associated with long-term morbidity in mothers and lifelong morbidities for their children, ranging from cerebral palsy and cognitive delay in preterm infants, to hypertension, diabetes and obesity in adolescents and young adults. There are several processes that are critical for development of materno-fetal exchange, including establishing adequate perfusion of the placenta by maternal blood, and the formation of the placental villous vascular tree. Recent studies provide persuasive evidence that placenta-derived extracellular vesicles (EVs) represent a significant intercellular communication pathway, and that they may play an important role in placental and endothelial cell (both fetal and maternal) function. These functions are known to be altered in PE. EVs can carry and transport a wide range of bioactive molescules that have potential to be used as biomarkers and therapeutic delivery tools for PE. EV content is often parent cell specific, thus providing an insight or “thumbprint” of the intracellular environment of the originating cell (e.g., human placenta). EV have been identified in plasma under both normal and pathological conditions, including PE. The concentration of EVs and their content in plasma has been reported to increase in association with disease severity and/or progression. Placenta-derived EVs have been identified in maternal plasma during normal pregnancy and PE pregnancies. They contain placenta-specific proteins and miRNAs and, as such, may be differentiated from maternally-derived EVs. The aim of this review, thus, is to describe the potential roles of EVs in preecmpatic pregnancies, focussing on EVs secreted from placental cells. The biogenesis, specificity of placental EVs, and methods used to characterise EVs in the context of PE pregnancies will be also discussed.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Alijotas-Reig J, Palacio-Garcia C, Farran-Codina I, Ruiz-Romance M, Llurba E, Vilardell-Tarres M (2012) Circulating cell-derived microparticles in severe preeclampsia and in fetal growth restriction. Am J Reprod Immunol 67:140–151
Ally AI, Horrobin DF (1980) Thromboxane A2 in blood vessel walls and its physiological significance: relevance to thrombosis and hypertension. Prostaglandins Med 4:431–438
Anderson UD, Gram M, Akerstrom B, Hansson SR (2015) First trimester prediction of preeclampsia. Curr Hypertens Rep 17:584
Armant DR, Kilburn BA, Petkova A, Edwin SS, Duniec-Dmuchowski ZM, Edwards HJ, Romero R, Leach RE (2006) Human trophoblast survival at low oxygen concentrations requires metalloproteinase-mediated shedding of heparin-binding EGF-like growth factor. Development 133:751–759
Auer J, Camoin L, Guillonneau F, Rigourd V, Chelbi ST, Leduc M, Laparre J, Mignot TM, Vaiman D (2010) Serum profile in preeclampsia and intra-uterine growth restriction revealed by iTRAQ technology. J Proteome 73:1004–1017
Bairoch A (2000) The ENZYME database in 2000. Nucleic Acids Res 28:304–305
Baker M (2015) Reproducibility crisis: blame it on the antibodies. Nature 521:274–276
Bakhti A, Vaiman D (2011) Prevention of gravidic endothelial hypertension by aspirin treatment administered from the 8th week of gestation. Hypertens Res 34:1116–1120
Benyo DF, Smarason A, Redman CW, Sims C, Conrad KP (2001) Expression of inflammatory cytokines in placentas from women with preeclampsia. J Clin Endocrinol Metab 86:2505–2512
Biró E, Lok CA, Hack CE, van der Post JA, Schaap MC, Sturk A, Nieuwland R (2007) Cell-derived microparticles and complement activation in preeclampsia versus normal pregnancy. Placenta 28:928–935
Biró O, Fóthi Á, Alasztics B, Nagy B, Orbán TI, Rigó J Jr (2019) Circulating exosomal and Argonaute-bound microRNAs in preeclampsia. Gene 692:138–144
Blumenstein M, McMaster MT, Black MA, Wu S, Prakash R, Cooney J, McCowan LM, Cooper GJ, North RA (2009) A proteomic approach identifies early pregnancy biomarkers for preeclampsia: novel linkages between a predisposition to preeclampsia and cardiovascular disease. Proteomics 9:2929–2945
Boisramé-Helms J, Meziani F, Sananès N, Boisramé T, Langer B, Schneider F, Ragot T, Andriantsitohaina R, Tesse A (2015) Detrimental arterial inflammatory effect of microparticles circulating in preeclamptic women: ex vivo evaluation in human arteries. Fundam Clin Pharmacol 29:450–461
Burton GJ, Jauniaux E (2015) What is the placenta? Am J Obstet Gynecol 213:S6.e1
Burton GJ, Woods AW, Jauniaux E, Kingdom JC (2009) Rheological and physiological consequences of conversion of the maternal spiral arteries for uteroplacental blood flow during human pregnancy. Placenta 30:473–482
Campello E, Spiezia L, Radu CM, Dhima S, Visentin S, Valle FD, Tormene D, Woodhams B, Cosmi E, Simioni P (2015) Circulating microparticles in umbilical cord blood in normal pregnancy and pregnancy with preeclampsia. Thromb Res 136:427–431
Caruso S, Poon IKH (2018) Apoptotic cell-derived extracellular vesicles: more than just debris. Front Immunol 9:1486–1486
Chang X, Yao J, He Q, Liu M, Duan T, Wang K (2018) Exosomes from women with preeclampsia induced vascular dysfunction by delivering sFlt (soluble Fms-like tyrosine kinase)-1 and sEng (soluble endoglin) to endothelial cells. Hypertension 72:1381–1390
Chaparro A, Gaedechens D, Ramírez V, Zuñiga E, Kusanovic JP, Inostroza C, Varas-Godoy M, Silva K, Salomon C, Rice G, Illanes SE (2016) Placental biomarkers and angiogenic factors in oral fluids of patients with preeclampsia. Prenat Diagn 36:476–482
Chargaff E, West R (1946) The biological significance of the thromboplastic protein of blood. J Biol Chem 166:189–197
Chelbi ST, Mondon F, Jammes H, Buffat C, Mignot TM, Tost J, Busato F, Gut I, Rebourcet R, Laissue P, Tsatsaris V, Goffinet F, Rigourd V, Carbonne B, Ferre F, Vaiman D (2007) Expressional and epigenetic alterations of placental serine protease inhibitors: SERPINA3 is a potential marker of preeclampsia. Hypertension 49:76–83
Chen Y, Huang Y, Jiang R, Teng Y (2012) Syncytiotrophoblast-derived microparticle shedding in early-onset and late-onset severe pre-eclampsia. Int J Gynaecol Obstet 119:234–238
Colombo M, Raposo G, Théry C (2014) Biogenesis, secretion, and intercellular interactions of exosomes and other extracellular vesicles. Annu Rev Cell Dev Biol 30:255–289
Cuckle H, von Dadelszen P, Ghidini A (2013) Current controversies in prenatal diagnosis 4: pregnancy complications due to placental vascular disease (pre-eclampsia, FGR): are we ready for prevention? Prenat Diagn 33:17–20
Di Simone N, Meroni PL, D'Asta M, Di Nicuolo F, D’Alessio MC, Caruso A (2007) Pathogenic role of anti-beta2-glycoprotein I antibodies on human placenta: functional effects related to implantation and roles of heparin. Hum Reprod Update 13:189–196
Downing JW, Ramasubramanian R, Johnson RF, Minzter BH, Paschall RL, Sundell HW, Engelhardt B, Lewis R (2004) Hypothesis: selective phosphodiesterase-5 inhibition improves outcome in preeclampsia. Med Hypotheses 63:1057–1064
Dragovic RA, GP Collett PH, Ferguson DJP, Redman CW, Sargent IL, Tannetta DS (2015) Isolation of syncytiotrophoblast microvesicles and exosomes and their characterisation by multicolour flow cytometry and fluorescence nanoparticle tracking analysis. Methods 87:64–74
Dutta S, Lai A, Scholz-Romero K, Shiddiky MJA, Yamauchi Y, Mishra JS, Rice GE, Hyett J, Kumar S, Salomon C (2020) Hypoxia-induced small extracellular vesicle proteins regulate proinflammatory cytokines and systemic blood pressure in pregnant rats. Clin Sci (Lond) 134:593–607
Elfeky O, Longo S, Lai A, Rice GE, Salomon C (2017) Influence of maternal BMI on the exosomal profile during gestation and their role on maternal systemic inflammation. Placenta 50:60–69
Ellis R, Katerelos M, Choy SW, Cook N, Lee M, Paizis K, Pell G, Walker S, Power DA, Mount PF (2019) Increased expression and phosphorylation of 6-phosphofructo-2-kinase/fructose-2,6-bisphosphatase isoforms in urinary exosomes in pre-eclampsia. J Transl Med 17:60
Euser AG, Metz TD, Allshouse AA, Heyborne KD (2016) Low-dose aspirin for pre-eclampsia prevention in twins with elevated human chorionic gonadotropin. J Perinatol 36:601–605
Friedman AM, Cleary KL (2014) Prediction and prevention of ischemic placental disease. Semin Perinatol 38:177–182
Gilani SI, Weissgerber TL, Garovic VD, Jayachandran M (2016) Preeclampsia and extracellular vesicles. Curr Hypertens Rep 18:1–11
Gilani SI, Anderson UD, Jayachandran M, Weissgerber TL, Zand L, White WM, Milic N, Suarez MLG, Vallapureddy RR, Nääv Å, Erlandsson L, Lieske JC, Grande JP, Nath KA, Hansson SR, Garovic VD (2017) Urinary extracellular vesicles of podocyte origin and renal injury in preeclampsia. J Am Soc Nephrol 28:3363–3372
Gilbert JS, Ryan MJ, LaMarca BB, Sedeek M, Murphy SR, Granger JP (2008) Pathophysiology of hypertension during preeclampsia: linking placental ischemia with endothelial dysfunction. Am J Physiol Heart Circ Physiol 294:H541–H550
Gill M, Motta-Mejia C, Kandzija N, Cooke W, Zhang W, Cerdeira AS, Bastie C, Redman C, Vatish M (2019) Placental syncytiotrophoblast-derived extracellular vesicles carry active NEP (Neprilysin) and are increased in preeclampsia. Hypertension 73:1112–1119
González-Quintero VH, Smarkusky LP, Jiménez JJ, Mauro LM, Jy W, Hortsman LL, O'Sullivan MJ, Ahn YS (2004) Elevated plasma endothelial microparticles: preeclampsia versus gestational hypertension. Am J Obstet Gynecol 191:1418–1424
Goswami D, Tannetta DS, Magee LA, Fuchisawa A, Redman CW, Sargent IL, von Dadelszen P (2006) Excess syncytiotrophoblast microparticle shedding is a feature of early-onset pre-eclampsia, but not normotensive intrauterine growth restriction. Placenta 27:56–61
Granger JP, Alexander BT, Llinas MT, Bennett WA, Khalil RA (2002) Pathophysiology of preeclampsia: linking placental ischemia/hypoxia with microvascular dysfunction. Microcirculation 9:147–160
Han C, Wang C, Chen Y, Wang J, Xu X, Hilton T, Cai W, Zhao Z, Wu Y, Li K, Houck K, Liu L, Sood AK, Wu X, Xue F, Li M, Dong JF, Zhang J (2019) Placenta-derived extracellular vesicles induce preeclampsia in mouse models. Haematologica 105(6):1686–1694
Helou A, Walker S, Stewart K, George J (2016) Management of pregnancies complicated by hypertensive disorders of pregnancy: could we do better? Aust N Z J Obstet Gynaecol 57(3):253–259
Hu CC, Katerelos M, Choy SW, Crossthwaite A, Walker SP, Pell G, Lee M, Cook N, Mount PF, Paizis K, Power DA (2018) Pre-eclampsia is associated with altered expression of the renal sodium transporters NKCC2, NCC and ENaC in urinary extracellular vesicles. PLoS One 13:e0204514
Jadli A, Ghosh K, Satoskar P, Damania K, Bansal V, Shetty S (2017) Combination of copeptin, placental growth factor and total annexin V microparticles for prediction of preeclampsia at 10-14 weeks of gestation. Placenta 58:67–73
Jan R, Chaudhry G-E-S (2019) Understanding apoptosis and apoptotic pathways targeted cancer therapeutics. Adv Pharm Bull 9(2):205–218. https://doi.org/10.15171/apb.2019.024. Epub 2019
Jia R, Li J, Rui C, Ji H, Ding H, Lu Y, De W, Sun L (2015) Comparative proteomic profile of the human umbilical cord blood exosomes between normal and preeclampsia pregnancies with high-resolution mass spectrometry. Cell Physiol Biochem 36:2299–2306
Johnstone RM, Adam M, Hammond JR, Orr L, Turbide C (1987) Vesicle formation during reticulocyte maturation. Association of plasma membrane activities with released vesicles (exosomes). J Biol Chem 262:9412–9420
Knight M, Redman CW, Linton EA, Sargent IL (1998) Shedding of syncytiotrophoblast microvilli into the maternal circulation in pre-eclamptic pregnancies. Br J Obstet Gynaecol 105:632–640
Kobayashi M, Rice GE, Tapia J, Mitchell MD, Salomon C (2014) Exosomes are fingerprints of originating cells: potential biomarkers for ovarian cancer. Res Rep Biochem 2014:101–109
Kohli S, Ranjan S, Hoffmann J, Kashif M, Daniel EA, Al-Dabet MM, Bock F, Nazir S, Huebner H, Mertens PR, Fischer KD, Zenclussen AC, Offermanns S, Aharon A, Brenner B, Shahzad K, Ruebner M, Isermann B (2016) Maternal extracellular vesicles and platelets promote preeclampsia via inflammasome activation in trophoblasts. Blood 128:2153–2164
Kowal J, Tkach M, Thery C (2014) Biogenesis and secretion of exosomes. Curr Opin Cell Biol 29:116–125
Levine L, Habertheuer A, Ram C, Korutla L, Schwartz N, Hu RW, Reddy S, Freas A, Zielinski PD, Harmon J, Molugu SK, Parry S, Vallabhajosyula P (2020) Syncytiotrophoblast extracellular microvesicle profiles in maternal circulation for noninvasive diagnosis of preeclampsia. Sci Rep 10:6398
Lockwood CJ, Yen CF, Basar M, Kayisli UA, Martel M, Buhimschi I, Buhimschi C, Huang SJ, Krikun G, Schatz F (2008) Preeclampsia-related inflammatory cytokines regulate interleukin-6 expression in human decidual cells. Am J Pathol 172:1571–1579
Lok CA, Böing AN, Reitsma PH, van der Post JA, van Bavel E, Boer K, Sturk A, Nieuwland R (2006) Expression of inflammation-related genes in endothelial cells is not directly affected by microparticles from preeclamptic patients. J Lab Clin Med 147:310–320
Lok CA, Nieuwland R, Sturk A, Hau CM, Boer K, Vanbavel E, Vanderpost JA (2007) Microparticle-associated P-selectin reflects platelet activation in preeclampsia. Platelets 18:68–72
Lok CA, Böing AN, Sargent IL, Sooranna SR, van der Post JA, Nieuwland R, Sturk A (2008a) Circulating platelet-derived and placenta-derived microparticles expose Flt-1 in preeclampsia. Reprod Sci 15:1002–1010
Lok CA, Van Der Post JA, Sargent IL, Hau CM, Sturk A, Boer K, Nieuwland R (2008b) Changes in microparticle numbers and cellular origin during pregnancy and preeclampsia. Hypertens Pregnancy 27:344–360
Lok CA, Jebbink J, Nieuwland R, Faas MM, Boer K, Sturk A, Van Der Post JA (2009) Leukocyte activation and circulating leukocyte-derived microparticles in preeclampsia. Am J Reprod Immunol 61:346–359
Lok CA, Snijder KS, Nieuwland R, Van Der Post JA, de Vos P, Faas MM (2012) Microparticles of pregnant women and preeclamptic patients activate endothelial cells in the presence of monocytes. Am J Reprod Immunol 67:206–215
Lyall F, Myatt L (2002) The role of the placenta in pre-eclampsia: a workshop report. Placenta 23(Suppl A):S142–S145
Marques FK, Campos FM, Filho OA, Carvalho AT, Dusse LM, Gomes KB (2012) Circulating microparticles in severe preeclampsia. Clin Chim Acta 414:253–258
McCoy S, Baldwin K (2009) Pharmacotherapeutic options for the treatment of preeclampsia. Am J Health Syst Pharm 66:337–344
McDonald SD, Malinowski A, Zhou Q, Yusuf S, Devereaux PJ (2008) Cardiovascular sequelae of preeclampsia/eclampsia: a systematic review and meta-analyses. Am Heart J 156(5):918–930. https://doi.org/10.1016/j.ahj.2008.06.042. Epub 2008 Oct 2
Meiri H, Sammar M, Herzog A, Grimpel YI, Fihaman G, Cohen A, Kivity V, Sharabi-Nov A, Gonen R (2014) Prediction of preeclampsia by placental protein 13 and background risk factors and its prevention by aspirin. J Perinat Med 42:591–601
Meziani F, Tesse A, David E, Martinez MC, Wangesteen R, Schneider F, Andriantsitohaina R (2006) Shed membrane particles from preeclamptic women generate vascular wall inflammation and blunt vascular contractility. Am J Pathol 169:1473–1483
Mikhailova VA, Ovchinnikova OM, Zainulina MS, Sokolov DI, Sel'kov SA (2014) Detection of microparticles of leukocytic origin in the peripheral blood in normal pregnancy and preeclampsia. Bull Exp Biol Med 157:751–756
Miller VM, Garovic VD, Bailey KR, Lahr BD, Mielke MM, White WM, Jayachandran M (2016) Pregnancy history and blood-borne microvesicles in middle aged women with and without coronary artery calcification. Atherosclerosis 253:150–155
Moro L, Bardají A, Macete E, Barrios D, Morales-Prieto DM, España C, Mandomando I, Sigaúque B, Dobaño C, Markert UR, Benitez-Ribas D, Alonso PL, Menéndez C, Mayor A (2016) Placental microparticles and microRNAs in pregnant women with Plasmodium falciparum or HIV infection. PLoS One 11:e0146361
Motawi TMK, Sabry D, Maurice NW, Rizk SM (2018) Role of mesenchymal stem cells exosomes derived microRNAs; miR-136, miR-494 and miR-495 in pre-eclampsia diagnosis and evaluation. Arch Biochem Biophys 659:13–21
Motta-Mejia C, Kandzija N, Zhang W, Mhlomi V, Cerdeira AS, Burdujan A, Tannetta D, Dragovic R, Sargent IL, Redman CW, Kishore U, Vatish M (2017) Placental vesicles carry active endothelial nitric oxide synthase and their activity is reduced in preeclampsia. Hypertension 70:372–381
Nwanodi OB (2016) Preeclampsia-eclampsia adverse outcomes reduction: the preeclampsia-eclampsia checklist. Healthcare (Basel) 4:26
O’Brien M, Baczyk D, Kingdom JC (2017) Endothelial dysfunction in severe preeclampsia is mediated by soluble factors, rather than extracellular vesicles. Sci Rep 7:5887
Pai CH, Yen CT, Chen CP, Yu IS, Lin SW, Lin SR (2016) Lack of thromboxane synthase prevents hypertension and fetal growth restriction after high salt treatment during pregnancy. PLoS One 11(3): e0151617
Pan BT, Johnstone RM (1983) Fate of the transferrin receptor during maturation of sheep reticulocytes in vitro: selective externalization of the receptor. Cell 33:967–978
Pan BT, Teng K, Wu C, Adam M, Johnstone RM (1985) Electron microscopic evidence for externalization of the transferrin receptor in vesicular form in sheep reticulocytes. J Cell Biol 101:942–948
Paulick MG, Bertozzi CR (2008) The glycosylphosphatidylinositol anchor: a complex membrane-anchoring structure for proteins. Biochemistry 47:6991–7000
Petrozella L, Mahendroo M, Timmons B, Roberts S, McIntire D, Alexander JM (2012) Endothelial microparticles and the antiangiogenic state in preeclampsia and the postpartum period. Am J Obstet Gynecol 207:140.e20–140.e26
Pillay P, Maharaj N, Moodley J, Mackraj I (2016) Placental exosomes and pre-eclampsia: maternal circulating levels in normal pregnancies and, early and late onset pre-eclamptic pregnancies. Placenta 46:18–25
Pillay P, Vatish M, Duarte R, Moodley J, Mackraj I (2019) Exosomal microRNA profiling in early and late onset preeclamptic pregnant women reflects pathophysiology. Int J Nanomedicine 14:5637–5657
Poon LC, Shennan A, Hyett JA, Kapur A (2019) The International Federation of Gynecology and Obstetrics (FIGO) initiative on pre‐eclampsia: a pragmatic guide for first‐trimester screening and prevention. Int J Gynecol Obstet 145:1–33. https://doi.org/10.1002/ijgo.12802. First published: 20 May 2019
Poutsiaka DD, Schroder EW, Taylor DD, Levy EM, Black PH (1985) Membrane vesicles shed by murine melanoma cells selectively inhibit the expression of Ia antigen by macrophages. J Immunol 134:138–144
Rader BA (2017) Alkaline phosphatase, an unconventional immune protein. eCollection 8:897
Raghupathy R (2013) Cytokines as key players in the pathophysiology of preeclampsia. Med Princ Pract 22(Suppl 1):8–19
Redman CW, Sargent IL (2009) Placental stress and pre-eclampsia: a revised view. Placenta 30(Suppl A):S38–S42
Reslan OM, Khalil RA (2010) Molecular and vascular targets in the pathogenesis and management of the hypertension associated with preeclampsia. Cardiovasc Hematol Agents Med Chem 8:204–226
Rolnik DL, O’Gorman N, Fiolna M, van den Boom D, Nicolaides KH, Poon LC (2015) Maternal plasma cell-free DNA in the prediction of pre-eclampsia. Ultrasound Obstet Gynecol 45:106–111
Salem M, Kamal S, El Sherbiny W, Abdel Aal AA (2015) Flow cytometric assessment of endothelial and platelet microparticles in preeclampsia and their relation to disease severity and Doppler parameters. Hematology 20:154–159
Salomon O, Katz BZ, Dardik R, Livnat T, Steinberg DM, Achiron R, Seligsohn U (2009) Plasma levels of microparticles at 24 weeks of gestation do not predict subsequent pregnancy complications. Fertil Steril 92:682–687
Salomon C, Guanzon D, Scholz-Romero K, Longo S, Correa P, Illanes SE, Rice GE (2017) Placental exosomes as early biomarker of preeclampsia: potential role of exosomal microRNAs across gestation. J Clin Endocrinol Metab 102:3182–3194
Sammar M, Dragovic R, Meiri H, Vatish M, Sharabi-Nov A, Sargent I, Redman C, Tannetta D (2018) Reduced placental protein 13 (PP13) in placental derived syncytiotrophoblast extracellular vesicles in preeclampsia - a novel tool to study the impaired cargo transmission of the placenta to the maternal organs. Placenta 66:17–25
Sandrim VC, Luizon MR, Palei AC, Tanus-Santos JE, Cavalli RC (2016) Circulating microRNA expression profiles in pre-eclampsia: evidence of increased miR-885-5p levels. BJOG 123:2120–2128
Schwartzman RA, Cidlowski JA (1993) Apoptosis: the biochemistry and molecular biology of programmed cell death. Endocr Rev 14(2):133–151. https://doi.org/10.1210/edrv-14-2-133
Sellers MM, Stallone JN (2008) Sympathy for the devil: the role of thromboxane in the regulation of vascular tone and blood pressure. Am J Physiol Heart Circ Physiol 294:H1978–H1986
Seravalli V, Grimpel YI, Meiri H, Blitzer M, Baschat AA (2016) Relationship between first-trimester serum placental protein-13 and maternal characteristics, placental Doppler studies and pregnancy outcome. J Perinat Med 44:543–549
Sokolov DI, Ovchinnikova OM, Korenkov DA, Viknyanschuk AN, Benken KA, Onokhin KV, Selkov SA (2016) Influence of peripheral blood microparticles of pregnant women with preeclampsia on the phenotype of monocytes. Transl Res 170:112–123
Tan KH, Tan SS, Sze SK, Lee WK, Ng MJ, Lim SK (2014) Plasma biomarker discovery in preeclampsia using a novel differential isolation technology for circulating extracellular vesicles. Am J Obstet Gynecol 211:380.e1–380.13
Tang Y, Chen Y, Nursalim Y, Groom K, Hickey A, Chamley L, Chen Q (2020) Endoplasmic reticulum stress occurs in association with the extrusion of toxic extracellular vesicles from human placentae treated with antiphospholipid antibodies. Clin Sci (Lond) 134:459–472
Tong M, Cheng SB, Chen Q, DeSousa J, Stone PR, James JL, Chamley LW, Sharma S (2017a) Aggregated transthyretin is specifically packaged into placental nano-vesicles in preeclampsia. Sci Rep 7:6694
Tong M, Johansson C, Xiao F, Stone PR, James JL, Chen Q, Cree LM, Chamley LW (2017b) Antiphospholipid antibodies increase the levels of mitochondrial DNA in placental extracellular vesicles: alarming for preeclampsia. Sci Rep 7:16556
Vanwijk MJ, Svedas E, Boer K, Nieuwland R, Vanbavel E, Kublickiene KR (2002) Isolated microparticles, but not whole plasma, from women with preeclampsia impair endothelium-dependent relaxation in isolated myometrial arteries from healthy pregnant women. Am J Obstet Gynecol 187:1686–1693
Vaughan JE, Walsh SW, Ford GD (2006) Thromboxane mediates neutrophil superoxide production in pregnancy. Am J Obstet Gynecol 195:1415–1420
Walsh SW (2004) Eicosanoids in preeclampsia. Prostaglandins Leukot Essent Fatty Acids 70:223–232
Walsh SW (1985) Preeclampsia: an imbalance in placental prostacyclin and thromboxane production. Am J Obstet Gynecol 152:335–340
Xiong ZH, Wei J, Lu MQ, Jin MY, Geng HL (2018) Protective effect of human umbilical cord mesenchymal stem cell exosomes on preserving the morphology and angiogenesis of placenta in rats with preeclampsia. Biomed Pharmacother 105:1240–1247
Xu J, Jia X, Gu Y, Lewis DF, Gu X, Wang Y (2017) Vitamin D reduces oxidative stress-induced procaspase-3/ROCK1 activation and MP release by placental trophoblasts. J Clin Endocrinol Metab 102:2100–2110
Yusuf K, Smith SD, Levy R, Schaiff WT, Wyatt SM, Sadovsky Y, Nelson DM (2001) Thromboxane A2 limits differentiation and enhances apoptosis of cultured human trophoblasts. Pediatr Res 50:203–209
Zarovni N, Corrado A, Guazzi P, Zocco D, Lari E, Radano G, Muhhina J, Fondelli C, Gavrilova J, Chiesi A (2015) Integrated isolation and quantitative analysis of exosome shuttled proteins and nucleic acids using immunocapture approaches. Methods 87:46–58
Zhao S, Gu Y, Lewis DF, Wang Y (2008) Predominant basal directional release of thromboxane, but not prostacyclin, by placental trophoblasts from normal and preeclamptic pregnancies. Placenta 29:81–88
Zhao M, Li Y, Xu L, Hickey A, Groom K, Stone PR, Chamley LW, Chen Q (2017) Melatonin prevents preeclamptic sera and antiphospholipid antibodies inducing the production of reactive nitrogen species and extrusion of toxic trophoblastic debris from first trimester placentae. Placenta 58:17–24
Acknowledgements
CS is supported by The Lions Medical Research Foundation, National Health and Medical Research Council (NHMRC; 1195451), and Fondo Nacional de Desarrollo Científico y Tecnológico (FONDECYT 1170809). CS and GD are supported by the Royal Brisbane and Women’s Hopsital foundation. CP has a PhD scholarship from CONICYT PFCHA / Doctorado Becas Chile/2018 – 72190513.
Conflict of Interest
The authors have nothing to declare.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Palma, C. et al. (2021). Extracellular Vesicles and Preeclampsia: Current Knowledge and Future Research Directions. In: Mathivanan, S., Fonseka, P., Nedeva, C., Atukorala, I. (eds) New Frontiers: Extracellular Vesicles. Subcellular Biochemistry, vol 97. Springer, Cham. https://doi.org/10.1007/978-3-030-67171-6_18
Download citation
DOI: https://doi.org/10.1007/978-3-030-67171-6_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-67170-9
Online ISBN: 978-3-030-67171-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)