Abstract
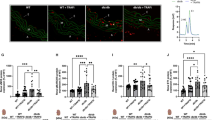
Diabetes is an established risk factor for ischemic stroke, but the associated molecular mechanisms remain to be fully elucidated. This study investigated the role of plasma and platelet microRNAs and their targeting proteins in the activation of platelets and their association with the occurrence of ischemic stroke in patients with type 2 diabetes mellitus (T2DM). Results showed that the expressions of platelet and plasma miR-144 and miR-223 were significantly altered in T2DM patients with or without ischemic stroke compared to that in healthy controls, but these changes were more significant in T2DM patients with ischemic stroke. The expressions of P2Y12 and IRS-1 as well as phosphorylation levels of IRS-1, PI3K, and Akt in platelets were significantly altered in T2DM patients with or without ischemic stroke. The expression of platelet miR-144 and miR-223 significantly correlated with their plasma levels, P2Y12 and IRS-1 expression, blood glucose concentration, and platelet activation rate. High glucose concentration significantly elevated P-selectin, miR-144 and P2Y12 expression and significantly reduced miR-223 and IRS-1 expression in UT-7 cells. Overexpression of miR-223 and blocking of miR-144 expression significantly normalized the effects of high glucose concentration in UT-7 cells. In conclusion, hyperglycemia may activate platelets through miR-144 and miR-223 to downregulate IRS-1 and upregulate P2Y12 expression in the platelets of T2DM patients through an IRS-1–PI3K–Akt signaling. Low platelet and plasma miR-223 expression in addition to high platelet and plasma miR-144 expression are risk factors for ischemic stroke in T2DM patients.





Similar content being viewed by others
References
Gerrits, A. J., Koekman, C. A., van Haeften, T. W., & Akkerman, J. W. (2010). Platelet tissue factor synthesis in type 2 diabetic patients is resistant to inhibition by insulin. Diabetes, 59, 1487–1495.
Nakagami, H., Kaneda, Y., Ogihara, T., & Morishita, R. (2005). Endothelial dysfunction in hyperglycemia as a trigger of atherosclerosis. Current Diabetes Review, 1, 59–63.
Burchfiel, C. M., Curb, J. D., Rodriguez, B. L., Abbott, R. D., Chiu, D., & Yano, K. (1994). Glucose intolerance and 22-year stroke incidence. The Honolulu Heart Program. Stroke, 25, 951–957.
Ferreiro, J. L., Gomez-Hospital, J. A., & Angiolillo, D. J. (2010). Platelet abnormalities in diabetes mellitus. Diabetes and Vascular Disease Research, 7, 251–259.
Todd Cade, W. (2008). Diabetes-related microvascular and macrovascular diseases in the physical therapy setting. Physical Therapy, 88, 1322–1335.
Kirshner, H. S. (2009). Differentiating ischemic stroke subtypes: Risk factors and secondary prevention. Journal of the Neurological Sciences, 279, 1–8.
Jackson, S. P., Nesbitt, W. S., & Kulkarni, S. (2003). Signaling events underlying thrombus formation. Journal of Thrombosis and Haemostasis, 1, 1602–1612.
Dorsam, R. T., & Kunapuli, S. P. (2004). Central role of the P2Y12 receptor in platelet activation. Journal of Clinical Investigation, 113, 340–345.
Jin, J., Quinton, T. M., Zhang, J., Rittenhouse, S. E., & Kunapuli, S. P. (2002). Adenosine diphosphate (ADP)-induced thromboxane A(2) generation in human platelets requires coordinated signaling through integrin alpha(IIb)beta(3) and ADP receptors. Blood, 99, 193–198.
Brozinick, J. T, Jr, Roberts, B. R., & Dohm, G. L. (2003). Defective signaling through Akt-2 and -3 but not Akt-1 in insulin-resistant human skeletal muscle: Potential role in insulin resistance. Diabetes, 52, 935–941.
Mardilovich, K., Pankratz, S. L., & Shaw, L. M. (2009). Expression and function of the insulin receptor substrate proteins in cancer. Cell Communication and Signaling, 7, 14.
Bruchova, H., Merkerova, M., & Prchal, J. T. (2008). Aberrant expression of microRNA in polycythemia vera. Haematologica, 93, 1009–1016.
Bartel, D. P. (2009). MicroRNAs: target recognition and regulatory functions. Cell, 136, 215–233.
Evans, D. J., Jackman, L. E., Chamberlain, J., Crosdale, D. J., Judge, H. M., Jetha, K., et al. (1992). Platelet P2Y(12) receptor influences the vessel wall response to arterial injury and thrombosis. Circulation, 119, 116–122.
Hartwig, J. H. (1992). Mechanisms of actin rearrangements mediating platelet activation. Journal of Cell Biology, 118, 1421–1442.
Kondratov, R. V., Chernov, M. V., Kondratova, A. A., Gorbacheva, V. Y., Gudkov, A. V., & Antoch, M. P. (2003). BMAL1-dependent circadian oscillation of nuclear CLOCK: Posttranslational events induced by dimerization of transcriptional activators of the mammalian clock system. Genes & Development, 17, 1921–1932.
Li, J., Rohailla, S., Gelber, N., Rutka, J., Sabah, N., Gladstone, R. A., et al. (2014). MicroRNA-144 is a circulating effector of remote ischemic preconditioning. Basic Research in Cardiology, 109, 423.
Duan, X., Zhan, Q., Song, B., Zeng, S., Zhou, J., Long, Y., et al. (2014). Detection of platelet microRNA expression in patients with diabetes mellitus with or without ischemic stroke. Journal of Diabetes and Its Complications, 28, 705–710.
Landry, P., Plante, I., Ouellet, D. L., Perron, M. P., Rousseau, G., & Provost, P. (2009). Existence of a microRNA pathway in anucleate platelets. Nature Structural & Molecular Biology, 16, 961–966.
Karolina, D. S., Armugam, A., Tavintharan, S., Wong, M. T., Lim, S. C., Sum, C. F., & Jeyaseelan, K. (2011). MicroRNA 144 impairs insulin signaling by inhibiting the expression of insulin receptor substrate 1 in type 2 diabetes mellitus. PLoS One, 6, e22839.
Michelson, A. D., Barnard, M. R., Krueger, L. A., Frelinger, A. L, 3rd, & Furman, M. I. (2000). Evaluation of platelet function by flow cytometry. Methods, 21, 259–270.
Mitchell, P. S., Parkin, R. K., Kroh, E. M., Fritz, B. R., Wyman, S. K., Pogosova-Agadjanyan, E. L., et al. (2008). Circulating microRNAs as stable blood-based markers for cancer detection. Proceedings of the National Academy of Science USA, 105, 10513–10518.
Bai, M., Zhu, X., Zhang, Y., Zhang, S., Zhang, L., Xue, L., et al. (2012). Abnormal hippocampal BDNF and miR-16 expression is associated with depression-like behaviors induced by stress during early life. PLoS One, 7, e46921.
Zhang, X., Li, Y., Huang, Q., Wang, H., Yan, B., Dewhirst, M. W., & Li, C. Y. (2003). Increased resistance of tumor cells to hyperthermia mediated by integrin-linked kinase. Clinical Cancer Research, 9, 1155–1160.
Ferreira, I. A., Mocking, A. I., Feijge, M. A., Gorter, G., van Haeften, T. W., Heemskerk, J. W., & Akkerman, J. W. (2006). Platelet inhibition by insulin is absent in type 2 diabetes mellitus. Arteriosclerosis, Thrombosis, and Vascular Biology, 26, 417–422.
Angiolillo, D. J., Bernardo, E., Zanoni, M., Vivas, D., Capranzano, P., Malerba, G., et al. (2011). Impact of insulin receptor substrate-1 genotypes on platelet reactivity and cardiovascular outcomes in patients with type 2 diabetes mellitus and coronary artery disease. Journal of the American College of Cardiology, 58, 30–39.
Dangwal, S., & Thum, T. (2012). MicroRNAs in platelet biogenesis and function. Thrombosis and Haemostasis, 108, 599–604.
Zimmerman, G. A., & Weyrich, A. S. (2008). Signal-dependent protein synthesis by activated platelets: New pathways to altered phenotype and function. Arteriosclerosis, Thrombosis, and Vascular Biology, 28, s17–s24.
Zampetaki, A., Kiechl, S., Drozdov, I., Willeit, P., Mayr, U., Prokopi, M., et al. (2010). Plasma microRNA profiling reveals loss of endothelial miR-126 and other microRNAs in type 2 diabetes. Circulation Research, 107, 810–817.
Ferreira, I. A., Mocking, A. I., Feijge, M. A., Gorter, G., van Haeften, T. W., Heemskerk, J. W., & Akkerman, J. W. (2006). Platelet inhibition by insulin is absent in type 2 diabetes mellitus. Arteriosclerosis, Thrombosis, and Vascular Biology, 26, 417–422.
Shantsila, E., Kamphuisen, P. W., & Lip, G. Y. (2010). Circulating microparticles in cardiovascular disease: Implications for atherogenesis and atherothrombosis. Journal of Thrombosis and Haemostasis, 8, 2358–2368.
Diehl, P., Fricke, A., Sander, L., Stamm, J., Bassler, N., Htun, N., et al. (2012). Microparticles: Major transport vehicles for distinct microRNAs in circulation. Cardiovascular Research, 93, 633–644.
Acknowledgments
This study was supported by Changsha Science and Technology Plan (K0902033-31), Hunan Science and Technology Plan (2009FJ3209), National Hi-tech Project of China (2007AA021809), Key Project of International Cooperation, Ministry of Science and Technology of China (2010DFB30300), and National Natural Science Foundation of China (No: 81272193).
Conflict of interest
The authors declared no conflict of interest.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Yang, S., Zhao, J., Chen, Y. et al. Biomarkers Associated with Ischemic Stroke in Diabetes Mellitus Patients. Cardiovasc Toxicol 16, 213–222 (2016). https://doi.org/10.1007/s12012-015-9329-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-015-9329-8