Abstract
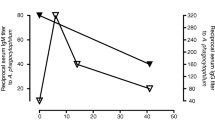
Histoplasma capsulatum var. capsulatum is a thermally dimorphic fungus that causes histoplasmosis. Fungal hemagglutination activity and cases of reactive hemophagocytic syndrome (RHS) have been reported in the disseminated form of disease. In the present study, soluble components of H. capsulatum var. capsulatum have been investigated for hemagglutinin activity and the capacity to induce hemophagocytosis in the mouse system. To analyze hemagglutinating activity, mouse red blood cells (RBC) (1% v/v in PBS) were incubated (37°C, 1 h) with cell-free antigen (CFAg) from H. capsulatum var. capsulatum (isolate IMT/HC128) (RBC-CFAg) or previously heated CFAg (56°C, 30 min) (RBC-hCFAg) or as control with PBS (RBC-PBS). Hemophagocytosis was analyzed by incubating BALB/c mouse peritoneal phagocytic cells (5 × 106 cells) with syngeneic RBC, sensitized or not with CFAg. In addition, mouse polyclonal antibodies were raised against syngeneic RBC-CFAg (anti-RBC-CFAg) and used to analyze CFAg chromatographic fractions (Sephadex G75/120) by immunoenzymatic assay (ELISA). Hemagglutinin activity was observed with RBC-CFAg, but not with RBC-hCFAg or RBC. Also, hemophagocytosis was observed with RBC-CFAg, but not with RBC. The anti-RBC-CFAg antibodies reacted with CFAg fractions corresponding to a molecular mass (MM) higher than 150 kDa. In conclusion, the yeast form of H. capsulatum var. capsulatum releases thermolabile soluble components with hemagglutinin activity and it has been demonstrated for the first time that soluble components of the same fungus induce syngeneic hemophagocytosis in the in vitro mouse system. Also, indirect analysis with antibodies suggests that high-MM components (>150 kDa) are responsible for the interaction with RBC.



Similar content being viewed by others
References
Reyes-Montes MDR, Taylor ML, Curiel-Quesada E, et al. Current knowledge on the strain typing of the pathogenic fungus Histoplasma capsulatum var. capsulatum: a review of the findings. Rev Iberoam Micol. 2000;17:121–6.
Wheat LJ, Cloud G, Johnson PC, et al. Clearance of fungal burden during treatment of disseminated histoplasmoses with liposomal amphotericin B versus itraconazole. Antimicrob Agents Chemother. 2001;45:2354–7.
Leimann BCQ, Pizzini CV, Muniz MM, et al. Histoplasmosis in a Brazilian center clinical forms and laboratory tests. Rev Iberoamer Micol. 2005;22:141–6.
Eissenberg LG, Goldman WE. Histoplasma variation and adaptive strategies for parasitism: new perspectives on histoplasmosis. Clin Microbiol Rev. 1991;4:411–21.
Wheat LJ, Sarosi G, McKinsey D, Hamill R, et al. Practice guidelines for the management of patients with histoplasmosis. Infectious Diseases Society of America. Clin Infect Dis. 2000;30:688–95.
Rachid A, Rezende LS, Moura SF, et al. A case study of disseminated histoplasmosis linked to common variable immunodeficiency. Braz J Infect Dis. 2003;7:268–72.
Tsuda H. Hemophagocytic syndrome (HPS) in children and adults. Int J Hematol. 1997;65:215–26.
Wang Z, Duarte AG, Scnadig J. Fatal reactive hemophagocytosis related to disseminated histoplasmosis with endocarditis: an unusual case diagnosed at autopsy. South Med Assoc. 2006;100:208–11.
Guiot HM, Bertrán-Pasarell J, Tormos LM, et al. Ileal perforation and reactive hemophagocytic syndrome in a patient with disseminated histoplasmosis: the role of real-time polymerase chain reaction in the diagnosis and successful treatment with amphotericin B lipid complex. Diagn Microbiol Infect Dis. 2007;57:429–33.
Janka G, Imashuku S, Elinder G, et al. Infection and malignancy-associated hemophagocytic syndromes. Secondary hemophagocytic lymphohistiocytosis. Hematol Oncol Clin North Am. 1998;12:435–44.
Fisman DN. Hemophagocytic syndromes and infection. Emerg Infect Dis. 2000;6:601–8.
Janka G, Stadt UZ. Familial and acquired hemophagocytic lymphohistiocytosis. Hematol Am Soc Hematol Educ Program. 2005;5:82–8.
Taylor ML, Duarte-Escalante E, Pérez A, et al. Histoplasma capsulatum yeast cells attach and agglutinate human erythrocytes. Med Mycol. 2004;42:287–92.
Sá-Nunes A, Medeiros AI, Nicolete R, et al. Efficacy of cell-free antigens in evaluating cell immunity and inducing protection in a murine model of histoplasmosis. Microbes Infect. 2005;7:584–92.
Camargo ZP, Taborda CP, Rodrigues EG, Travassos LR. The use of cell-free antigens of Paracoccidioides brasiliensis in serological tests. J Med Vet Mycol. 1991;29:31–8.
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ. Protein measurement with the folin phenol reagent. J Biol Chem. 1951;193:265–75.
Fujiwara F, Hibbi S, Imashuku S. Hypercytokinemia and hemophagocytic syndrome. Am J Pediatr Hematol Oncol. 1993;15:92–8.
Ohga S, Maatsuzaki A, Nishizaki M. Inflammatory cytokines in virus-associated hemophagocytic syndrome: interferon gamma as a sensitive indicator of disease activity. Am J Pediatr Hematol Oncol. 1993;15:291–8.
Durkin MM, Connolly PAA, Wheat LJ. Comparison of radioimmunoassay and enzyme-linked immunoassay methods for detection of Histoplasma capsulatum var. capsulatum antigen. J Clin Microbiol. 1997;35:2252–5.
Wheat LJ, Garringer T, Brizendine E, Connolly P. Diagnosis of histoplasmosis by antigen detection based upon experience at the histoplasmosis reference laboratory. Diagn Microbiol Infect Dis. 2002;43:29–37.
Bullock WE, Artz RP, Bhathena D, Tung KS. Histoplasmosis. Arch Intern Med. 1979;139:700–2.
Kauffman CA. Histoplasmosis: a clinical and laboratory update. Clin Microbiol Rev. 2007;20:115–32.
Acknowledgments
This work was supported by Fundação Araucária/PR, Fundação de Apoio ao Ensino, Pesquisa e Extensão (FAEP/UEL), Coordenação de Aperfeiçoamento de Pessoal de Nivel Superior (CAPES) and Japan International Cooperation Agency (JICA). The authors thank Timothy J. C. Roberts for the correction of the English text.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vivan, R.H.F., Leonello, P.C., Nagashima, L.A. et al. Soluble Components of Histoplasma Capsulatum var. Capsulatum have Hemagglutinin Activity and Induce Syngeneic Hemophagocytosis In Vitro. Mycopathologia 169, 151–157 (2010). https://doi.org/10.1007/s11046-009-9243-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-009-9243-3