Abstract
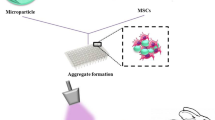
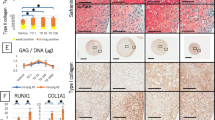
With the application of tissue engineering to tissue regeneration, additional new complexes have been made in response to the challenge of cartilage-injury repair. This study was performed to construct a rat precartilaginous stem cells-based scaffold of self-assembling peptides RADA16-I/PLGA-PLL (poly-l-lysine coated PLGA) as extracellular matrix loading the NLS-TAT as a peptide-based carrier for a plasmid DNA containing hTGFβ3. After composites were cultured for 1, 2, 3 and 4 weeks, respectively, the results showed that the levels of chondrogenic-related gene expression were higher in the experimental group with and hTGFβ3 gene by reverse transcription-polymerase chain reaction, and with higher histochemical and immunohistochemical expression. hTGFβ3 protein expression had increased at 4 weeks based on western blot analysis. The results of this study show that a complex may be a suitable scaffold for cartilage repair and offer a strategy for tissue regeneration through the use of tissue engineering.
Graphical Abstract








Similar content being viewed by others
References
Mollon B, Kandel R, Chahal J, Theodoropoulos J. The clinical status of cartilage tissue regeneration in humans. Osteoarthr Cartil. 2013;21(12):1824–33. doi:10.1016/j.joca.2013.08.024.
Veronesi F, Maglio M, Tschon M, Aldini NN, Fini M. Adipose-derived mesenchymal stem cells for cartilage tissue engineering: state-of-the-art in in vivo studies. J Biomed Mater Res A. 2014;102(7):2448–66. doi:10.1002/jbm.a.34896.
Chen JL, Duan L, Zhu W, Xiong J, Wang D. Extracellular matrix production in vitro in cartilage tissue engineering. J Transl Med. 2014;12:88. doi:10.1186/1479-5876-12-88.
Perez RA, Won JE, Knowles JC, Kim HW. Naturally and synthetic smart composite biomaterials for tissue regeneration. Adv Drug Deliv Rev. 2013;65(4):471–96. doi:10.1016/j.addr.2012.03.009.
Benders KE, van Weeren PR, Badylak SF, Saris DB, Dhert WJ, Malda J. Extracellular matrix scaffolds for cartilage and bone regeneration. Trends Biotechnol. 2013;31(3):169–76. doi:10.1016/j.tibtech.2012.12.004.
Bhardwaj N, Kundu SC. Chondrogenic differentiation of rat MSCs on porous scaffolds of silk fibroin/chitosan blends. Biomaterials. 2012;33(10):2848–57. doi:10.1016/j.biomaterials.2011.12.028.
Zhang K, Zhang Y, Yan S, Gong L, Wang J, Chen X, et al. Repair of an articular cartilage defect using adipose-derived stem cells loaded on a polyelectrolyte complex scaffold based on poly(l-glutamic acid) and chitosan. Acta Biomater. 2013;9(7):7276–88. doi:10.1016/j.actbio.2013.03.025.
Nojehdehian H, Moztarzadeh F, Baharvand H, Nazarian H, Tahriri M. Preparation and surface characterization of poly-l-lysine-coated PLGA microsphere scaffolds containing retinoic acid for nerve tissue engineering: in vitro study. Colloids Surf B Biointerfaces. 2009;73(1):23–9. doi:10.1016/j.colsurfb.2009.04.029.
Dai W, Kawazoe N, Lin X, Dong J, Chen G. The influence of structural design of PLGA/collagen hybrid scaffolds in cartilage tissue engineering. Biomaterials. 2010;31(8):2141–52. doi:10.1016/j.biomaterials.2009.11.070.
Wu YC, Shaw SY, Lin HR, Lee TM, Yang CY. Bone tissue engineering evaluation based on rat calvaria stromal cells cultured on modified PLGA scaffolds. Biomaterials. 2006;27(6):896–904. doi:10.1016/j.biomaterials.2005.07.002.
Reyes R, Delgado A, Solis R, Sanchez E, Hernandez A, San Roman J, et al. Cartilage repair by local delivery of transforming growth factor-beta1 or bone morphogenetic protein-2 from a novel, segmented polyurethane/polylactic-co-glycolic bilayered scaffold. J Biomed Mater Res A. 2014;102(4):1110–20. doi:10.1002/jbma.34769.
Reyes R, Delgado A, Sanchez E, Fernandez A, Hernandez A, Evora C. Repair of an osteochondral defect by sustained delivery of BMP-2 or TGFbeta1 from a bilayered alginate-PLGA scaffold. J Tissue Eng Regen Med. 2014;8(7):521–33. doi:10.1002/term.1549.
Caplan MR, Schwartzfarb EM, Zhang S, Kamm RD, Lauffenburger DA. Control of self-assembling oligopeptide matrix formation through systematic variation of amino acid sequence. Biomaterials. 2002;23(1):219–27.
Cormier AR, Pang X, Zimmerman MI, Zhou HX, Paravastu AK. Molecular structure of RADA16-I designer self-assembling peptide nanofibers. ACS Nano. 2013;7(9):7562–72. doi:10.1021/nn401562f.
Ye Z, Zhang H, Luo H, Wang S, Zhou Q, Du X, et al. Temperature and pH effects on biophysical and morphological properties of self-assembling peptide RADA16-I. J Pept Sci. 2008;14(2):152–62. doi:10.1002/psc.988.
Maude S, Ingham E, Aggeli A. Biomimetic self-assembling peptides as scaffolds for soft tissue engineering. Nanomedicine (Lond). 2013;8(5):823–47. doi:10.2217/nnm.13.65.
Zhang S, Holmes TC, DiPersio CM, Hynes RO, Su X, Rich A. Self-complementary oligopeptide matrices support mammalian cell attachment. Biomaterials. 1995;16(18):1385–93.
Cormier AR, Lopez-Majada JM, Alamo RG, Paravastu AK. Distinct solid and solution state self-assembly pathways of RADA16-I designer peptide. J Pept Sci. 2013;19(8):477–84. doi:10.1002/psc.2524.
Nagai Y, Unsworth LD, Koutsopoulos S, Zhang S. Slow release of molecules in self-assembling peptide nanofiber scaffold. J Control Release. 2006;115(1):18–25. doi:10.1016/j.jconrel.2006.06.031.
Koutsopoulos S, Unsworth LD, Nagai Y, Zhang S. Controlled release of functional proteins through designer self-assembling peptide nanofiber hydrogel scaffold. Proc Natl Acad Sci U S A. 2009;106(12):4623–8. doi:10.1073/pnas.0807506106.
Dasgupta A, Mondal JH, Das D. Peptide hydrogels. Rsc Advances. 2013;3(24):9117–49.
Guo T, Zhao J, Chang J, Ding Z, Hong H, Chen J, et al. Porous chitosan-gelatin scaffold containing plasmid DNA encoding transforming growth factor-beta1 for chondrocytes proliferation. Biomaterials. 2006;27(7):1095–103. doi:10.1016/j.biomaterials.2005.08.015.
Lee CH, Cook JL, Mendelson A, Moioli EK, Yao H, Mao JJ. Regeneration of the articular surface of the rabbit synovial joint by cell homing: a proof of concept study. Lancet. 2010;376(9739):440–8. doi:10.1016/s0140-6736(10)60668-x.
Kim SE, Park JH, Cho YW, Chung H, Jeong SY, Lee EB, et al. Porous chitosan scaffold containing microspheres loaded with transforming growth factor-beta1: implications for cartilage tissue engineering. J Control Release. 2003;91(3):365–74.
Tang QO, Shakib K, Heliotis M, Tsiridis E, Mantalaris A, Ripamonti U, et al. TGF-beta3: a potential biological therapy for enhancing chondrogenesis. Expert Opin Biol Ther. 2009;9(6):689–701. doi:10.1517/14712590902936823.
Levick JR. A method for estimating macromolecular reflection by human synovium, using measurements of intra-articular half lives. Ann Rheum Dis. 1998;57(6):339–44.
Ignatovich IA, Dizhe EB, Pavlotskaya AV, Akifiev BN, Burov SV, Orlov SV, et al. Complexes of plasmid DNA with basic domain 47-57 of the HIV-1 Tat protein are transferred to mammalian cells by endocytosis-mediated pathways. J Biol Chem. 2003;278(43):42625–36. doi:10.1074/jbc.M301431200.
Coles DJ, Yang S, Esposito A, Mitchell D, Minchin RF, Toth I. The synthesis and characterisation of a novel dendritic system for gene delivery. Tetrahedron. 2007;63(49):12207–14.
Yang S, Coles DJ, Esposito A, Mitchell DJ, Toth I, Minchin RF. Cellular uptake of self-assembled cationic peptide-DNA complexes: multifunctional role of the enhancer chloroquine. J Control Release. 2009;135(2):159–65. doi:10.1016/j.jconrel.2008.12.015.
Robinson D, Hasharoni A, Cohen N, Yayon A, Moskowitz RM, Nevo Z. Fibroblast growth factor receptor-3 as a marker for precartilaginous stem cells. Clin Orthop Relat Res. 1999;(367 Suppl):S163–75. doi:10.1097/00003086-199910001-00018.
Zhang S, Chen A, Hu W, Li M, Liao H, Zhu W, et al. Immunological purification of rat precartilaginous stem cells and construction of the immortalized cell strain. Arch Orthop Trauma Surg. 2008;128(11):1339–44. doi:10.1007/s00402-008-0571-4.
Guo X, Chu X, Li W, Pan Q, You H. Chondrogenic effect of precartilaginous stem cells following NLS-TAT cell penetrating peptide-assisted transfection of eukaryotic hTGFbeta3. J Cell Biochem. 2013;114(11):2588–94. doi:10.1002/jcb.24606.
Cheng H, Chen A, You H. Immunomagnetic indirect positive sorting of precartilaginous stem cells from neonatal rat. J Huazhong Univ Sci Technolog Med Sci. 2006;26(6):723–4.
Kisiday J, Jin M, Kurz B, Hung H, Semino C, Zhang S, et al. Self-assembling peptide hydrogel fosters chondrocyte extracellular matrix production and cell division: implications for cartilage tissue repair. Proc Natl Acad Sci U S A. 2002;99(15):9996–10001. doi:10.1073/pnas.142309999.
Jeong JH, Kim SW, Park TG. A new antisense oligonucleotide delivery system based on self-assembled ODN-PEG hybrid conjugate micelles. J Control Release. 2003;93(2):183–91.
Kong HJ, Kim ES, Huang YC, Mooney DJ. Design of biodegradable hydrogel for the local and sustained delivery of angiogenic plasmid DNA. Pharm Res. 2008;25(5):1230–8. doi:10.1007/s11095-007-9526-7.
de Crombrugghe B, Lefebvre V, Behringer RR, Bi W, Murakami S, Huang W. Transcriptional mechanisms of chondrocyte differentiation. Matrix Biol. 2000;19(5):389–94.
You H, Chen A, Liu T, Wang M, Zhang G. Construction of eukaryotic expression plasmid of hTGF-beta3 and its inducing effect on differentiation of precartilaginous stem cells into chondroblasts. J Huazhong Univ Sci Technolog Med Sci. 2011;31(4):524–9. doi:10.1007/s11596-011-0484-2.
Acknowledgments
This work was supported by Grants from the Nature Science Foundation of Hubei Province (No. 2014060101010048) and National Natural Science Foundation of China (No. 81541020).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Pan, Q., Li, W., Yuan, X. et al. Chondrogenic effect of cell-based scaffold of self-assembling peptides/PLGA-PLL loading the hTGFβ3 plasmid DNA. J Mater Sci: Mater Med 27, 19 (2016). https://doi.org/10.1007/s10856-015-5631-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-015-5631-z