Abstract
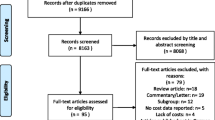
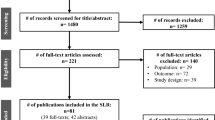
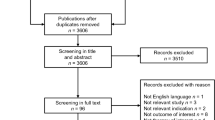
The aim of this study is to perform a systematic review of the costing methodological approaches adopted by published cost-of-illness (COI) studies. A systematic review was performed to identify cost-of-illness studies of heart failure published between January 2003 and September 2015 via computerized databases such as Pubmed, Wiley Online, Science Direct, Web of Science, and Cumulative Index to Nursing and Allied Health Literature (CINAHL). Costs reported in the original studies were converted to 2014 international dollars (Int$). Thirty five out of 4972 studies met the inclusion criteria. Nineteen out of the 35 studies reported the costs as annual cost per patient, ranging from Int$ 908.00 to Int$ 84,434.00, while nine studies reported costs as per hospitalization, ranging from Int$ 3780.00 to Int$ 34,233.00. Cost of heart failure increased as condition of heart failure worsened from New York Heart Association (NYHA) class I to NYHA class IV. Hospitalization cost was found to be the main cost driver to the total health care cost. The annual cost of heart failure ranges from Int$ 908 to Int$ 40,971 per patient. The reported cost estimates were inconsistent across the COI studies, mainly due to the variation in term of methodological approaches such as disease definition, epidemiological approach of study, study perspective, cost disaggregation, estimation of resource utilization, valuation of unit cost components, and data sources used. Such variation will affect the reliability, consistency, validity, and relevance of the cost estimates across studies.



Similar content being viewed by others
References
Mendez GF, Cowie MR (2001) The epidemiological features of heart failure in developing countries: A review of the literature. Int J Cardiol 80:213–219
Ambrosy AP, Fonarow GC, Butler J, Chioncel O, Greene SJ, Vaduganathan M, Nodari S, Lam CS, Sato N, Shah AN (2014) The global health and economic burden of hospitalizations for heart failure: Lessons learned from hospitalized heart failure registries. J Am Coll Cardiol 63:1123–1133
Mosterd A, Hoes A, De Bruyne M, Deckers J, Linker D, Hofman A, Grobbee D (1999) Prevalence of heart failure and left ventricular dysfunction in the general population; the Rotterdam study. Eur Heart J 20:447–455
Redfield MM, Jacobsen SJ, Burnett Jr JC, Mahoney DW, Bailey KR, Rodeheffer RJ (2003) Burden of systolic and diastolic ventricular dysfunction in the community: Appreciating the scope of the heart failure epidemic. JAMA 289:194–202
Roger VL, Go AS, Lloyd-Jones DM, Benjamin EJ, Berry JD, Borden WB, Bravata DM, Dai S, Ford ES, Fox CS (2012) Heart disease and stroke statistics—2012 update a report from the American Heart Association. Circulation 125:e2–e220
Reyes EB, Ha J-W, Firdaus I, Ghazi AM, Phrommintikul A, Sim D, QN V, Siu CW, Yin W-H, Cowie MR (2016) Heart failure across Asia: Same healthcare burden but differences in organization of care. Int J Cardiol 223:163–167
Nieminen MS, Harjola V-P (2005) Definition and epidemiology of acute heart failure syndromes. Am J Cardiol 96:5–10
Ho KK, Pinsky JL, Kannel WB, Levy D, Pitt B (1993) The epidemiology of heart failure: The Framingham study. J Am Coll Cardiol 22:A6–A13
Haldeman GA, Croft JB, Giles WH, Rashidee A (1999) Hospitalization of patients with heart failure: National Hospital Discharge Survey, 1985 to 1995. Am Heart J 137:352–360
United Nations Department of Economic and Social Affairs Population Division. World population ageing 2015. ST/ESA/SER.A/390 2015. http://www.un.org/en/development/desa/population/publications/pdf/ageing/WPA2015_Report.pdf. Accessed 1 Aug 2016
Blecker S, Paul M, Taksler G, Ogedegbe G, Katz S (2013) Heart failure-associated hospitalizations in the United States. J Am Coll Cardiol 61:1259–1267
Chen J, Normand S-LT, Wang Y, Krumholz HM (2011) National and regional trends in heart failure hospitalization and mortality rates for Medicare beneficiaries, 1998–2008. JAMA 306:1669–1678
Lloyd-Jones D, Adams R, Carnethon M, De Simone G, Ferguson TB, Flegal K, Ford E, Furie K, Go A, Greenlund K (2009) Heart disease and stroke statistics—2009 update a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 119:e21–e181
Cleland J, Swedberg K, Follath F, Komajda M, Cohen-Solal A, Aguilar JC, Dietz R, Gavazzi A, Hobbs R, Korewicki J (2003) The EuroHeart failure survey programme—a survey on the quality of care among patients with heart failure in Europe. Eur Heart J 24:442–463
Berry C, Murdoch DR, McMurray JJ (2001) Economics of chronic heart failure. Eur J Heart Fail 3:283–291
Stewart S, Jenkins A, Buchan S, McGuire A, Capewell S, McMurray JJ (2002) The current cost of heart failure to the National Health Service in the UK. Eur J Heart Fail 4:361–371
Liao L, Allen LA, Whellan DJ (2008) Economic burden of heart failure in the elderly. PharmacoEconomics 26:447–462
Rosamond W, Flegal K, Friday G, Furie K, Go A, Greenlund K, Haase N, Ho M, Howard V, Kissela B, Kittner S, Lloyd-Jones D, McDermott M, Meigs J, Moy C, Nichol G, O'Donnell CJ, Roger V, Rumsfeld J, Sorlie P, Steinberger J, Thom T, Wasserthiel-Smoller S, Hong Y (2007) Heart disease and stroke statistics—2007 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 115:e69–171
Ng TP, Niti M (2003) Trends and ethnic differences in hospital admissions and mortality for congestive heart failure in the elderly in Singapore, 1991 to 1998. Heart 89:865–870
Feldman DE, Thivierge C, Guérard L, Déry V, Kapetanakis C, Lavoie G, Beck EJ (2001) Changing trends in mortality and admissions to hospital for elderly patients with congestive heart failure in Montreal. Can Med Assoc J 165:1033–1036
Ryden-Bergsten T, Andersson F (1999) The health care costs of heart failure in Sweden. J Intern Med 246:275–284
Bundkirchen A, Schwinger RH (2004) Epidemiology and economic burden of chronic heart failure. Eur Heart J Suppl 6:D57–D60
Jefferson T, Demicheli V, Mugford M (2000) Elementary economic evaluation in health care. BMJ Publishing Group, London
Clabaugh G, Ward MM (2008) Cost-of-illness studies in the United States: A systematic review of methodologies used for direct cost. Value Health 11:13–21
Molinier L, Bauvin E, Combescure C, Castelli C, Rebillard X, Soulié M, Daurès J-P, Grosclaude P (2008) Methodological considerations in cost of prostate cancer studies: A systematic review. Value Health 11:878–885
Costa N, Derumeaux H, Rapp T, Garnault V, Ferlicoq L, Gillette S, Andrieu S, Vellas B, Lamure M, Grand A (2012) Methodological considerations in cost of illness studies on Alzheimer disease. Heal Econ Rev 2:18
Bloom BS, Bruno DJ, Maman DY, Jayadevappa R (2001) Usefulness of US cost-of-illness studies in healthcare decision making. PharmacoEconomics 19:207–213
World Bank. Price level ratio of PPP conversion factor (GDP) to market exchange rate. http://data.worldbank.org/indicator/PA.NUS.PPPC.RF. Accessed 26 January 2016
World Health Organization. Choosing interventions that are cost effective (WHO-CHOICE). http://www.who.int/choice/costs/ppp/en/. Accessed 19 August 2017 2017
Drummond MF (2005) Methods for the economic evaluation of health care programmes, 3rd edn. Oxford University Press, New York
Larg A, Moss JR (2011) Cost-of-illness studies. PharmacoEconomics 29:653–671
Hunt SA, Baker DW, Chin MH, Cinquegrani MP, Feldman AM, Francis GS, Ganiats TG, Goldstein S, Gregoratos G, Jessup ML (2001) ACC/AHA guidelines for the evaluation and management of chronic heart failure in the adult: Executive summary. A report of the American College of Cardiology/American Heart Association task force on practice guidelines (committee to revise the 1995 guidelines for the evaluation and management of heart failure). J Am Coll Cardiol 38:2101–2113
World Health Organization. International Classification of Diseases (ICD). http://www.who.int/classifications/icd/en/. Accessed 16 Nov 2015
World Health Organization. WHO guide to identifying the economic consequences of disease and injury 2009. http://www.who.int/choice/publications/d_economic_impact_guide.pdf. Accessed 13 March 2016
Costa N, Derumeaux H, Rapp T, Garnault V, Ferlicoq L, Gillette S, Andrieu S, Vellas B, Lamure M, Grand A (2012) Methodological considerations in cost of illness studies on Alzheimer disease. Heal Econ Rev 2:1–12
Haddix AC, Teutsch SM, Corso PS (2003) Prevention effectiveness: A guide to decision analysis and economic evaluation, 2nd edn. Oxford University Press, New York
Luce BR, Wanning WG, Siegel J, Lipscomb J (1996) Estimating costs in cost-effectiveness analysis. Cost-effectiveness in Health and. Medicine 3:176–213
Koopmanschap MA, van Ineveld BM (1992) Towards a new approach for estimating indirect costs of disease. Soc Sci Med 34:1005–1010
Koopmanschap MA, Rutten FF (1996) A practical guide for calculating indirect costs of disease. PharmacoEconomics 10:460–466
Gafni A (1991) Willingness-to-pay as a measure of benefits: Relevant questions in the context of public decisionmaking about health care programs. Med Care 29:1246–1252
Begley CE, Annegers JF, Lairson DR, Reynolds TF (1999) Methodological issues in estimating the cost of epilepsy. Epilepsy Res 33:39–55
Pagano E, Brunetti M, Tediosi F, Garattini L (1999) Costs of diabetes. PharmacoEconomics 15:583–595
Whellan DJ, Greiner MA, Schulman KA, Curtis LH (2010) Costs of inpatient care among Medicare beneficiaries with heart failure, 2001 to 2004. Circ Cardiovasc Qual Outcomes 3:33–40
Hauptman PJ, Swindle J, Burroughs TE, Schnitzler MA (2008) Resource utilization in patients hospitalized with heart failure: Insights from a contemporary national hospital database. Am Heart J 155:978–985. e971
Dunlay SM, Shah ND, Shi Q, Morlan B, VanHouten H, Long KH, Roger VL (2011) Lifetime costs of medical care after heart failure diagnosis. Circ Cardiovasc Qual Outcomes 4:68–75
Wang G, Zhang Z, Ayala C, Wall HK, Fang J (2010) Costs of heart failure-related hospitalizations in patients aged 18 to 64 years. Am J Manag Care 16:769–776
Corrao G, Ghirardi A, Ibrahim B, Merlino L, Maggioni AP (2014) Burden of new hospitalization for heart failure: A population-based investigation from Italy. Eur J Heart Fail 16:729–736
Voigt J, Sasha John M, Taylor A, Krucoff M, Reynolds MR, Michael Gibson C (2014) A reevaluation of the costs of heart failure and its implications for allocation of health resources in the United States. Clin Cardiol 37:312–321
Bogner HR, Miller SD, de Vries HF, Chhatre S, Jayadevappa R (2010) Assessment of cost and health resource utilization for elderly patients with heart failure and diabetes mellitus. J Card Fail 16:454–460
Joshi AV, D'Souza AO, Madhavan SS (2004) Differences in hospital length-of-stay, charges, and mortality in congestive heart failure patients. Congest Heart Fail 10:76–84
Claes N, Jacobs N, Vijgen J (2008) Impact of heart failure on hospital activity and healthcare costs in Belgium. J Med Econ 11:71–79
Bharmal M, Gemmen E, Zyczynski T, Linnstaedt A, Kenny D, Marelli C (2008) Resource utilisation, charges and mortality following hospital inpatient admission for congestive heart failure among the elderly in the US. J Med Econ 11:397–414
Korves C, Eldar-Lissai A, McHale J, Lafeuille M-H, Hwa Ong S, Sheng Duh M (2012) Resource utilization and costs following hospitalization of patients with chronic heart failure in the US. J Med Econ 15:925–937
Lagu T, Krumholz HM, Dharmarajan K, Partovian C, Kim N, Mody PS, Li SX, Strait KM, Lindenauer PK (2013) Spending more, doing more, or both? An alternative method for quantifying utilization during hospitalizations. J Hosp Med 8:373–379
Ziaeian B, Sharma PP, Yu T-C, Johnson KW, Fonarow GC (2015) Factors associated with variations in hospital expenditures for acute heart failure in the United States. Am Heart J 169:282–289 e215
Czech M, Opolski G, Zdrojewski T, Dubiel JS, Wizner B, Bolisęga D, Fedyk-Łukasik M, Grodzicki T (2012) The costs of heart failure in Poland from the public payer’s perspective. Polish programme assessing diagnostic procedures, treatment and costs in patients with heart failure in randomly selected outpatient clinics and hospitals at different levels of care: POLKARD. Kardiol Pol 71:224–232
Wijeysundera HC, Austin PC, Wang X, Bennell MC, Abrahamyan L, Ko DT, JV T, Krahn M (2014) The effect of multidisciplinary heart failure clinic characteristics on 1-year postdischarge health care costs: A population-based study. Med Care 52:272–279
Stålhammar J, Stern L, Linder R, Sherman S, Parikh R, Ariely R, Deschaseaux C, Wikström G (2014) The burden of preserved ejection fraction heart failure in a real-world Swedish patient population. J Med Econ 17:43–51
Kuwabara K, Matsuda S, Anan M, Fushimi K, Ishikawa KB, Horiguchi H, Hayashida K, Fujimori K (2010) Difference in resource utilization between patients with acute and chronic heart failure from Japanese administrative database. Int J Cardiol 141:254–259
Sözmen K, Pekel Ö, Yılmaz TS, Şahan C, Ceylan A, Güler E, Korkmaz E, Ünal B (2015) Determinants of inpatient costs of angina pectoris, myocardial infarction, and heart failure in a university hospital setting in Turkey. Anatol J Cardiol 15:325–333
Neumann T, Biermann J, Neumann A, Wasem J, Ertl G, Dietz R, Erbel R (2009) Heart failure: The commonest reason for hospital admission in Germany. Dtsch Arztebl Int 106:269–275
Tatari S, Soubra L, Tamim H, Akhras K, Kabbani S (2015) The economic impact of patients with heart failure on the Lebanese healthcare system. ESC. Heart Failure 2:178–183
Agvall B, Borgquist L, Foldevi M, Dahlström U (2005) Cost of heart failure in Swedish primary healthcare. Scand J Prim Health Care 23:227–232
Ogah OS, Stewart S, Onwujekwe OE, Falase AO, Adebayo SO, Olunuga T, Sliwa K (2014) Economic burden of heart failure: Investigating outpatient and inpatient costs in Abeokuta, Southwest Nigeria. PLoS One 9:e113032. https://doi.org/10.1371/journal.pone.0113032
Mejhert M, Lindgren P, Schill O, Edner M, Persson H, Kahan T (2013) Long term health care consumption and cost expenditure in systolic heart failure. Eur J Intern Med 24:260–265
Biermann J, Neumann T, Angermann CE, Düngen H-D, Erbel R, Herzog W, Maisch B, Müller-Tasch T, Özcelik C, Pankuweit S (2012) Resource use and costs in systolic heart failure according to disease severity: A pooled analysis from the German competence network heart failure. J Public Health 20:23–30
Russo MJ, Gelijns AC, Stevenson LW, Sampat B, Aaronson KD, Renlund DG, Ascheim DD, Hong KN, Oz MC, Moskowitz AJ (2008) The cost of medical management in advanced heart failure during the final two years of life. J Card Fail 14:651–658
Peters-Klimm F, Halmer A, Flessa S, Szecsenyi J, Ose D (2012) What drives the costs of heart failure care in Germany? A health services cost analysis. J Public Health 20:653–660
Araujo DV, Tavares LR, Veríssimo R, Ferraz MB, Mesquita ET (2005) Cost of heart failure in the unified health system. Arq Bras Cardiol 84:422–427
Delgado JF, Oliva J, Llano M, Pascual-Figal D, Grillo JJ, Comín-Colet J, Díaz B, de La Concha LM, Martí B, Peña LM (2014) Health care and nonhealth care costs in the treatment of patients with symptomatic chronic heart failure in Spain. Rev Esp Cardiol 67:643–650
Titler MG, Jensen GA, Dochterman JM, Xie XJ, Kanak M, Reed D, Shever LL (2008) Cost of hospital care for older adults with heart failure: medical, pharmaceutical, and nursing costs. Health Serv Res 43:635–655
Joo H, Fang J, Losby JL, Wang G (2015) Cost of informal caregiving for patients with heart failure. Am Heart J 169:142–148 e142
Parissis J, Athanasakis K, Farmakis D, Boubouchairopoulou N, Mareti C, Bistola V, Ikonomidis I, Kyriopoulos J, Filippatos G, Lekakis J (2015) Determinants of the direct cost of heart failure hospitalization in a public tertiary hospital. Int J Cardiol 180:46–49
Ondrackova B, Miklik R, Parenica J, Spinar J, Sticha M, Sulcova A (2009) In hospital costs of acute heart failure patients in the Czech Republic. Open Med 4:483–489
Liao L, Anstrom KJ, Gottdiener JS, Pappas PA, Whellan DJ, Kitzman DW, Aurigemma GP, Mark DB, Schulman KA, Jollis JG (2007) Long-term costs and resource use in elderly participants with congestive heart failure in the Cardiovascular Health Study. Am Heart J 153:245–252
Rihova B, Parenica J, Jarkovsky J, Miklik R, Sulcova A, Littnerova S, Felsoci M, Kala P, Spinar J (2013) Cardiology department hospitalization costs in patients with acute heart failure vary according to the etiology of the acute heart failure: Data from the AHEAD Core registry 2005–2009. Cor et Vasa 55:e7–e14
Liao L, Jollis JG, Anstrom KJ, Whellan DJ, Kitzman DW, Aurigemma GP, Mark DB, Schulman KA, Gottdiener JS (2006) Costs for heart failure with normal vs reduced ejection fraction. Arch Intern Med 166:112–118
Investigators SoLVD (1991) Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med 325:293–302
Segel JE (2006) Cost-of-illness studies—a primer. RTI-UNC Center of Excellence in Health Promotion Economics:1–39
Philbin EF, Mccullough PA, Dec GW, Disalvo TG (2001) Length of stay and procedure utilization are the major determinants of hospital charges for heart failure. Clin Cardiol 24:56–62
Braunschweig F, Cowie MR, Auricchio A (2011) What are the costs of heart failure? Europace 13:ii13–ii17
Greiner MA, Hammill BG, Fonarow GC, Whellan DJ, Eapen ZJ, Hernandez AF, Curtis LH (2012) Predicting costs among Medicare beneficiaries with heart failure. Am J Cardiol 109:705–711
McGowan B, Heerey A, Ryan M, Barry M (2000) Cost of treating heart failure in an Irish teaching hospital. Ir J Med Sci 169:241–244
Kjekshus J, Swedberg K, Snapinn S (1992) Effects of enalapril on long-term mortality in severe congestive heart failure. Am J Cardiol 69:103–107
Investigators S (1991) Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med 1991:293–302
Loeb HS, Johnson G, Henrick A, Smith R, Wilson J, Cremo R, Cohn JN (1993) Effect of enalapril, hydralazine plus isosorbide dinitrate, and prazosin on hospitalization in patients with chronic congestive heart failure. The V-HeFT VA Cooperative Studies Group Circulation 87:VI78–VI87
Group DI (1997, 1997) The effect of digoxin on mortality and morbidity in patients with heart failure. N Engl J Med:525–533
Uretsky BF, Young JB, Shahidi FE, Yellen LG, Harrison MC, Jolly MK, Group TPI (1993) Randomized study assessing the effect of digoxin withdrawal in patients with mild to moderate chronic congestive heart failure: Results of the PROVED trial. J Am Coll Cardiol 22:955–962
Packer M, Gheorghiade M, Young JB, Costantini PJ, Adams KF, Cody RJ, Smith LK, Van Voorhees L, Gourley LA, Jolly MK (1993) Withdrawal of digoxin from patients with chronic heart failure treated with angiotensin-converting-enzyme inhibitors. N Engl J Med 329:1–7
Investigators C-I (1999) The cardiac insufficiency bisoprolol study II (CIBIS-II): A randomised trial. Lancet 353:9–13
Hodgson TA, Meiners MR (1982) Cost-of-illness methodology: a guide to current practices and procedures. The Milbank Memorial Fund Quarterly Health and. Society:429–462
Van den Berg B, Brouwer WB, Koopmanschap MA (2004) Economic valuation of informal care. Europe J Health Econ, formerly: HEPAC 5:36–45
McMurray J, Hart W, Rhodes G (1993) An evaluation of the cost of heart failure to the National Health Service in the UK. Br J Med Econ 6:91–98
Szucs TD (2000) The growing healthcare burden of CHF. J Renin-Angiotensin-Aldosterone Syst 1:2–6
Davey PG, Clarkson PB, McMahon A, MacDonald TM (1999) Costs associated with symptomatic systolic heart failure. PharmacoEconomics 16:399–407
McAlister FA, Stewart S, Ferrua S, McMurray JJ (2004) Multidisciplinary strategies for the management of heart failure patients at high risk for admission: A systematic review of randomized trials. J Am Coll Cardiol 44:810–819
Agvall B, Paulsson T, Foldevi M, Dahlström U, Alehagen U (2014) Resource use and cost implications of implementing a heart failure program for patients with systolic heart failure in Swedish primary health care. Int J Cardiol 176:731–738
Ledwidge M, Barry M, Cahill J, Ryan E, Maurer B, Ryder M, Travers B, Timmons L, McDonald K (2003) Is multidisciplinary care of heart failure cost-beneficial when combined with optimal medical care? Eur J Heart Fail 5:381–389
Ho Y-L, Hsu T-P, Chen C-P, Lee C-Y, Lin Y-H, Hsu R-B, Y-W W, Chou N-K, Lee C-M, Wang S-S (2007) Improved cost-effectiveness for management of chronic heart failure by combined home-based intervention with clinical nursing specialists. J Formos Med Assoc 106:313–319
Tsuyuki RT, Fradette M, Johnson JA, Bungard TJ, Eurich DT, Ashton T, Gordon W, Ikuta R, Kornder J, Mackay E (2004) A multicenter disease management program for hospitalized patients with heart failure. J Card Fail 10:473–480
Laramee AS, Levinsky SK, Sargent J, Ross R, Callas P (2003) Case management in a heterogeneous congestive heart failure population: A randomized controlled trial. Arch Intern Med 163:809–817
Harrison MB, Browne GB, Roberts J, Tugwell P, Gafni A, Graham ID (2002) Quality of life of individuals with heart failure: A randomized trial of the effectiveness of two models of hospital-to-home transition. Med Care 40:271–282
Jaarsma T, Halfens R, Abu-Saad HH, Dracup K, Gorgels T, Van Ree J, Stappers J (1999) Effects of education and support on self-care and resource utilization in patients with heart failure. Eur Heart J 20:673–682
Honeycutt AA, Segel JE, Hoerger TJ, Finkelstein EA (2009) Comparing cost-of-illness estimates from alternative approaches: an application to diabetes. Health Serv Res 44:303–320
Tunceli O, Wade R, Gu T, Bouchard JR, Aagren M, Luo W (2010) Cost of diabetes: Comparison of disease-attributable and matched cohort cost estimation methods. Curr Med Res Opin 26:1827–1834
Seuring T, Archangelidi O, Suhrcke M (2015) The economic costs of type 2 diabetes: A global systematic review. PharmacoEconomics 33:811–831
Goff DC Jr, Pandey DK, Chan FA, Ortiz C, Nichaman MZ (2000) Congestive heart failure in the united states: Is there more than meets the i(cd code)? The Corpus Christi Heart Project. Arch Intern Med 160:197–202. https://doi.org/10.1001/archinte.160.2.197
Quach S, Blais C, Quan H (2010) Administrative data have high variation in validity for recording heart failure. Can J Cardiol 26:e306–e312
Van Walraven C, Taljaard M, Bell CM, Etchells E, Zarnke KB, Stiell IG, Forster AJ (2008) Information exchange among physicians caring for the same patient in the community. Can Med Assoc J 179:1013–1018
Rutten FH, Cramer M-JM, Grobbee DE, Sachs AP, Kirkels JH, Lammers J-WJ, Hoes AW (2005) Unrecognized heart failure in elderly patients with stable chronic obstructive pulmonary disease. Eur Heart J 26:1887–1894
Auerbach AD, Hamel MB, Davis RB, Connors AF, Regueiro C, Desbiens N, Goldman L, Califf RM, Dawson NV, Wenger N (2000) Resource use and survival of patients hospitalized with congestive heart failure: Differences in care by specialty of the attending physician. Ann Intern Med 132:191–200
Riley GF (2009) Administrative and claims records as sources of health care cost data. Med Care 47:S51–S55
Ceratti A, France FR, Beguin C (2008) Health data quality improvement by comparing administrative medical data and billing data. Int J Med Inform 77:527–533
Fox KM, Reuland M, Hawkes WG, Hebel JR, Hudson J, Zimmerman SI, Kenzora J, Magaziner J (1998) Accuracy of medical records in hip fracture. J Am Geriatr Soc 46:745–750
Alqaisi F, Williams LK, Peterson EL, Lanfear DE (2009) Comparing methods for identifying patients with heart failure using electronic data sources. BMC Health Serv Res 9:1
Schackman BR, Gold HT, Stone PW, Neumann PJ (2004) How often do sensitivity analyses for economic parameters change cost-utility analysis conclusions? PharmacoEconomics 22:293–300
Acknowledgements
All authors were involved in the conception and design of this work and approved the final manuscript. The preparation of this review did not receive any external funding or a grant. Y.P. Tan and C.H. Ng were the independent reviewers of the literature and were also responsible for study abstraction. Y.P. Tan and A.A. Shafie wrote the manuscript. A.A. Shafie supervised all systematic review activities and was responsible for the final manuscript review. A.A. Shafie is the overall guarantor for this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article did not contain any studies with human participants performed by any of the authors.
Informed consent
Informed consent was not needed as there was no human participant involved in this study.
Additional information
Key Points for Decision Makers
• The wide variation in cost estimates across different cost of illness studies of heart failure needs careful analysis and interpretation.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Shafie, A.A., Tan, Y.P. & Ng, C.H. Systematic review of economic burden of heart failure. Heart Fail Rev 23, 131–145 (2018). https://doi.org/10.1007/s10741-017-9661-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-017-9661-0