Abstract
Purpose
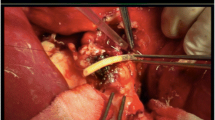
Bile duct (BD) complications continue to be the “Achilles’ heel” of liver transplantation, and the utilization of bile duct drainage is still on debate. We describe the results of a less invasive rubber trancystic biliary drainage (TBD) compared to a standard silicone T-tube (TT).
Methods
The transplanted patients (n = 248), over a period of 5 years with a TBD (n = 20), were matched 1:2 with control patients with a TT (n = 40). Primary end points were the overall incidence of BD complications and graft and patient survival. Secondary end points included the complications after the drainage removal.
Results
Although the bile duct leakage rates were not significantly different between both groups, the TT group had a significantly higher rate of overall 1-year BD stenosis (40 versus 10 %) (p = 0.036). Three-year patient/graft survival rates were 83.2/80.1 and 84.4/84.4 % for the TT and TBD groups, respectively. The postoperative BD complications, after drainage removal (peritonitis and stenosis), were significantly reduced (p = 0.011) with the use of a TBD.
Conclusion
The use of rubber TBD in liver transplant recipients does not increase the number of BD complications compared to the T-tube. Furthermore, less BD anastomotic stenosis and post-removal complications were observed in the TBD group compared to the TT group.

Similar content being viewed by others
References
Sotiropoulos GC, Sgourakis G, Radtke A, Molmenti EP, Goumas K, Mylona S et al (2009) Orthotopic liver transplantation: T-tube or not T-tube? Systematic review and meta-analysis of results. Transplantation 87(11):1672–1680
Scatton O, Meunier B, Cherqui D, Boillot O, Sauvanet A, Boudjema K et al (2001) Randomized trial of choledochocholedochostomy with or without a T tube in orthotopic liver transplantation. Ann Surg 233(3):432–437
Riediger C, Müller MW, Michalski CW, Hüser N, Schuster T, Kleeff J et al (2010) T-Tube or no T-tube in the reconstruction of the biliary tract during orthotopic liver transplantation: systematic review and meta-analysis. Liver Transpl 16(6):705–717
Sundaram V, Jones DT, Shah NH, de Vera ME, Fontes P, Marsh JW et al (2011) Posttransplant biliary complications in the pre- and post-model for end-stage liver disease era. Liver Transpl 17(4):428–435
Pascher A, Neuhaus P (2006) Biliary complications after deceased-donor orthotopic liver transplantation. J Hepatobiliary Pancreat Surg 13(6):487–496
Thethy S, Thomson BNJ, Pleass H, Wigmore SJ, Madhavan K, Akyol M et al (2004) Management of biliary tract complications after orthotopic liver transplantation. Clin Transplant 18(6):647–653
Escat J, Fourtanier G, Lacroix A, Anduze-Acher Y (1978) External drainage of the common bile duct. A new transcystic drain. Nouv Presse Med 7(19):1643–1644
Suc B, Escat J, Cherqui D, Fourtanier G, Hay JM, Fingerhut A et al (1998) Surgery vs endoscopy as primary treatment in symptomatic patients with suspected common bile duct stones: a multicenter randomized trial (French Associations for Surgical Research). Arch Surg 133(7):702–708
Narita M, Oussoultzoglou E, Jaeck D, Fuchschuber P, Rosso E, Pessaux P et al (2012) Two-stage hepatectomy for multiple bilobar colorectal liver metastases. Br J Surg. doi:10.1002/bjs.7580
Kobayashi T, Sato Y, Yamamoto S, Takeishi T, Oya H, Hirano K et al (2007) Characteristics of biliary reconstruction, using a T-tube, as compared to those with other methods, in left-lobe adult living-donor liver transplantation. J Hepatobiliary Pancreat Surg 14(2):177–182
Hotta T, Kobayashi Y, Taniguchi K, Johata K, Sahara M, Naka T et al (2003) Postoperative evaluation of C-tube drainage after hepatectomy. Hepatogastroenterology 50(50):485–490
Saidi RF, Elias N, Ko DS, Kawai T, Markmann J, Cosimi AB et al (2009) Biliary reconstruction and complications after living-donor liver transplantation. HPB (Oxford) 11(6):505–509
Innocenti F, Hepp J, Humeres R, Rios H, Suárez L, Zapata R et al (2004) Transcystic cholangiogram access via rubber band with early withdrawal after liver transplantation: a safe technique. Transplant Proc 36(6):1681–1682
Panaro F, Navarro F (2011) Optimizing outflow in piggyback liver transplantation without caval occlusion: the three-vein technique. Liver Transpl 17(6):742. doi:10.1002/lt.22290, author reply 743-4
Panaro F, Gallix B, Bouyabrine H, Ramos J, Addeo P, Testa G et al (2011) Liver transplantation and spontaneous neovascularization after arterial thrombosis: “the neovascularized liver”. Transpl Int 24(9):949–957
Audet M, Piardi T, Cag M, Navarro F, Ornis S, Cinqualbre C et al (2011) Hepatitis C recurrence after liver transplantation: has the HLA mismatching at individual loci a role? J Gastroenterol Hepatol 26(12):1772–1778. doi:10.1111/j.1440-1746.2011.06772.x
Weiss S, Schmidt SC, Ulrich F, Pascher A, Schumacher G, Stockmann M et al (2009) Biliary reconstruction using a side-to-side choledochocholedochostomy with or without T-tube in deceased donor liver transplantation: a prospective randomized trial. Ann Surg 250(5):766–771
Paes-Barbosa FC, Massarollo PC, Bernardo WM, Ferreira FG, Barbosa FK, Raslan M et al (2011) Systematic review and meta-analysis of biliary reconstruction techniques in orthotopic deceased donor liver transplantation. J Hepatobiliary Pancreat Sci 18(4):525–536
Shimoda M, Saab S, Morrisey M, Ghobrial RM, Farmer DG, Chen P et al (2001) A cost-effectiveness analysis of biliary anastomosis with or without T-tube after orthotopic liver transplantation. Am J Transplant 1(2):157–161
Akamatsu N, Sugawara Y, Hashimoto D (2011) Biliary reconstruction, its complications and management of biliary complications after adult liver transplantation: a systematic review of the incidence, risk factors and outcome. Transpl Int 24(4):379–392
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethics
Patients have given their informed consent and the study protocol has been approved by the institute’s committee on human research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Panaro, F., Glaise, A., Miggino, M. et al. Rubber transcystic drainage reduces the post-removal biliary complications in liver transplantation: a matched case–control study. Langenbecks Arch Surg 398, 169–176 (2013). https://doi.org/10.1007/s00423-012-0970-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-012-0970-4