Abstract
Objective
The objective of this study was to compare intravenous normal saline with and without 5 % dextrose on the course of labor in nulliparous women in active phase of spontaneous labor.
Study design
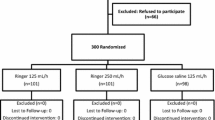
In a randomized controlled trial, term, nulliparous women with singleton pregnancy in active labor were randomized into one of two groups receiving either normal saline or normal saline alternating with 5 % dextrose at rate of 175 ml/h. The primary outcome was total length of labor from onset of study fluid in vaginally delivered women. Maternal and neonatal outcomes were also analyzed.
Results
Of 250 women enrolled, in vaginally delivered subjects, there was significant difference in the duration of labor (p = 0.0) and prolonged labor (p = 0.01), with favorable results for women in 5 % dextrose alternating with normal saline. No statistically significant differences were observed in the cesarean section rates between the groups. The cord pH was significantly higher in neonates born to women in 5 % dextrose alternating with normal saline infusion as compared to normal saline alone (p = 0.01), however, no neonate in the study had acidemia.
Conclusion
Administration of a 5 % dextrose solution alternating with normal saline is a better parenteral fluid for significantly decreasing duration of labor in term vaginally delivered nulliparous women in spontaneous active labor as compared to normal saline alone.


Similar content being viewed by others
References
Handa VL, Laros RK (1993) Active-phase arrest in labor: predictors of caesarean delivery in a nulliparous population. Obstet Gynecol 81:758–763
Garite TJ, Weeks J, Peters-Phair K, Pattillo C, Brewster WR (2000) A randomized control trial on the effect of increased intra-venous hydration on the course of labor in nulliparous women. Am J Obstet Gynecol 183:1544–1548
Eslamian L, Maroosi V, Pakneeyat Y (2006) Increased intravenous fluid intake and the course of labor in nulliparous women. Int J Gynaecol Obstet 93:102–105
Shrivastava VK, Garite TJ, Jenkis SM et al (2009) A randomized double blinded control trial comparing parenteral normal saline with and without dextrose on the course of labor in nulliparas. Am J Obstet Gynecol 200:379e1–379e6
Steingrimsdottir T, Ronquist G, Ulmsten U, Waldenstrom A (1995) Different energy metabolite pattern between uterine smooth muscle and striated rectus muscle in term pregnant women. Eur J Obstet Gynecol Reprod Biol 62:241–245
Steingrimsdottir T, Ronquist G, Ulstenn U (1993) Energy economy in pregnant human uterus at term: studies on arteriovenous differences in metabolites of carbohydrate, fat and nucleotides. Eur J Obstet Gynecol and Reprod Biol 51:209–215
Maughan RJ, Noakes TD (1991) Fluid replacement and exercise stress. A brief review of studies on fluid replacement and some guidelines for the athlete. Sports Med 12:16–31
Friedman EA (1978) Labor clinical evaluation and management, 2nd edn. Appleton Century Crofts, New York
Scheepers HCJ, Thans MCJ, de Jong PA et al (2002) A double blind, randomized, placebo controlled study on the influence of carbohydrate solution intake during labor. Br J Obstet Gynaecol 1091:78–81
Tarnow-Mordi WO, Shaw JC, Liu D, Gardner DA, Flynn FV (1981) Iatrogenic hyponatremia of the newborn due to maternal fluid overload: a prospective study. Br Med J (Clin Res Ed) 283:639–642
Johansson S, Lindow S, Kapadia H, Norman M (2002) Perinatal water intoxication due to excessive oral intake during labor. Acta Paedtr 91:811–814
West CR, Harding JE (2004) Maternal water intoxication as a cause of neonatal seizures. J Paediatr Child Health 40:709–710
Jamal A, Choobak N, Tabassomi F (2007) Intrapartum maternal glucose infusion and fetal acid base status. Int J Gynaecol Obstet 97:187–189
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sharma, C., Kalra, J., Bagga, R. et al. A randomized controlled trial comparing parenteral normal saline with and without 5 % dextrose on the course of labor in nulliparous women. Arch Gynecol Obstet 286, 1425–1430 (2012). https://doi.org/10.1007/s00404-012-2485-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-012-2485-1