Abstract
Introduction
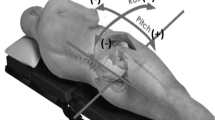
The position of the cup makes a major contribution to the success of total hip arthroplasty (THA). In conventional implantation of the prosthesis without navigation, the surgeon relies on the spatial position of the pelvis. However, iatrogenic manipulation of the pelvis during different surgical steps constantly changes the position of the pelvis during the operation. The position of the pelvis is substantial for the correct placement of the cup. The objective of this study was to investigate and visualize the course of this pelvic lift and correlate it to certain surgical steps.
Materials and methods
Pelvic lift was measured in 67 patients during implantation of a THA. This was done by measuring acceleration using the SensorLog app on a smartphone. It was placed on the patient’s contralateral anterior superior iliac spine and recorded the movement of the pelvis throughout the whole surgical procedure. The position of the pelvis was allocated to each of eight relevant surgical steps during the operation. These surgical steps were normed over the time axis and transferred to a diagram.
Results
We found an average pelvic lift displacement of up to 14.9° upon placement in the figure-of-four position. This lift is particularly critical when exposing the acetabulum, as the true cup position can be unconsciously influenced. Average values of between 5.6° and 6.9° were found here.
Conclusions
When implanting a THA in supine position, the pelvis is not fixed on the operating table. Rather, the side to be operated on is lifted to a greater or lesser degree, depending on the surgical step to be performed. The retractor traction immediately before cup implantation should be minimized. Nevertheless, it should be taken into account that anteversion of the cup implant in relation to the table plane is systematically higher than in relation to the pelvic entry plane.


Similar content being viewed by others
References
Harrison CL, Thomson AI, Cutts S, Rowe PJ, Riches PE (2014) Research synthesis of recommended acetabular cup orientations for total hip arthroplasty. J Arthroplasty 29:377–382
Nishii T, Sugano N, Miki H, Koyama T, Takao M, Yoshikawa H (2004) Influence of component positions on dislocation: computed tomographic evaluations in a consecutive series of total hip arthroplasty. J Arthroplasty 19:162–166
Kummer FJ, Shah S, Iyer S, DiCesare PE (1999) The effect of acetabular cup orientations on limiting hip rotation. J Arthroplasty 14:509–513
Patil S, Bergula A, Chen PC, Colwell CW, D’Lima DD (2003) Polyethylene wear and acetabular component orientation. J Bone Jt Surg Am 85-A Suppl 4:56–63
Walter WL, O’toole GC, Walter WK, Ellis A, Zicat BA (2007) Squeaking in ceramic-on-ceramic hips: the importance of acetabular component orientation. J Arthroplasty 22:496–503
Woo RY, Morrey BF (1982) Dislocations after total hip arthroplasty. J Bone Jt Surg Am 64:1295–1306
Tai SM, Munir S, Walter WL, Pearce SJ, Walter WK, Zicat BA (2015) Squeaking in large diameter ceramic-on-ceramic bearings in total hip arthroplasty. J Arthroplasty 30:282–285
Grammatopoulos G, Pandit HG, da Assunção R, Taylor A, McLardy-Smith P, De Smet KA, Murray DW, Gill HS (2014) Pelvic position and movement during hip replacement. Bone Jt J 96-B:876–883
Asayama I, Akiyoshi Y, Naito M, Ezoe M (2004) Intraoperative pelvic motion in total hip arthroplasty. J Arthroplasty 19:992–997
Kanazawa M, Nakashima Y, Ohishi M, Hamai S, Motomura G, Yamamoto T, Fukushi J-I, Ushijima T, Hara D, Iwamoto Y (2016) Pelvic tilt and movement during total hip arthroplasty in the lateral decubitus position. Mod Rheumatol 26:435–440
Callanan MC, Jarrett B, Bragdon CR, Zurakowski D, Rubash HE, Freiberg AA, Malchau H (2010) The John Charnley award: risk factors for cup malpositioning: quality improvement through a joint registry at a tertiary hospital. Clin Orthop Relat Res 469:319–329
Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR (1978) Dislocations after total hip-replacement arthroplasties. J Bone Jt Surg Am 60:217–220
Elkins JM, Callaghan JJ, Brown TD (2014) The 2014 Frank Stinchfield award: the “landing zone” for wear and stability in total hip arthroplasty is smaller than we thought: a computational analysis. Clin Orthop Relat Res 473:441–452
Danoff JR, Bobman JT, Cunn G, Murtaugh T, Gorroochurn P, Geller JA, Macaulay W (2016) Redefining the acetabular component safe zone for posterior approach total hip arthroplasty. J Arthroplasty 31:506–511
Renkawitz T, Weber M, Springorum H-R, Sendtner E, Woerner M, Ulm K, Weber T, Grifka J (2015) Impingement-free range of movement, acetabular component cover and early clinical results comparing ‘femur-first’ navigation and “conventional” minimally invasive total hip arthroplasty: a randomised controlled trial. Bone Jt J 97:890–898
Woerner M, Sendtner E, Springorum R, Craiovan B, Worlicek M, Renkawitz T, Grifka J, Weber M (2016) Visual intraoperative estimation of cup and stem position is not reliable in minimally invasive hip arthroplasty. Acta Orthop 87:225–230
Nakashima Y, Hirata M, Akiyama M, Itokawa T, Yamamoto T, Motomura G, Ohishi M, Hamai S, Iwamoto Y (2014) Combined anteversion technique reduced the dislocation in cementless total hip arthroplasty. Int Orthop 38:27–32
Weber M, Weber T, Woerner M, Craiovan B, Worlicek M, Winkler S, Grifka J, Renkawitz T (2015) The impact of standard combined anteversion definitions on gait and clinical outcome within one year after total hip arthroplasty. Int Orthop 39:2323–2333
Ezoe M, Naito M, Asayama I, Ishiko T, Fujisawa M (2005) Pelvic motion during total hip arthroplasty with translateral and posterolateral approaches. J Orthop Sci 10:167–172
Bauer R, Kerschbaumer F, Poisel S, Oberthaler W (1979) The transgluteal approach to the hip joint. Arch Orthop Trauma Surg 95:47–49
Acknowledgements
The authors would like to thank Hardi Hauk for taking and providing the photographs.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brodt, S., Nowack, D., Krakow, L. et al. Course of pelvic lift during total hip arthroplasty. Arch Orthop Trauma Surg 137, 129–133 (2017). https://doi.org/10.1007/s00402-016-2601-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-016-2601-y