Abstract
Introduction and hypothesis
Vaginal mesh kits are increasingly used in the management of pelvic organ prolapse. This study aimed to determine similarity of outcomes of the Anterior Prolift® with Perigee® systems for anterior compartment prolapse.
Methods
Consecutive women undergoing Perigee® or Anterior Prolift® for symptomatic stage 2 or greater anterior vaginal prolapse were prospectively evaluated. Main outcome measures included objective and subjective success rates, perioperative outcomes, patient satisfaction, and complications.
Results
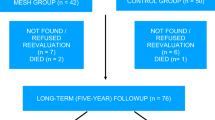
One hundred and six women (Prolift, 52; Perigee, 54) completed questionnaires, and 91 (Prolift, 46; Perigee, 45) were examined postoperatively. At follow-up (Prolift: median, 11.0; range, 5–23 months; Perigee: median, 11.5; range, 6–23 months), objective success rates (Prolift, 89%; Perigee, 80%; p = 0.23), subjective success rates (Prolift, 94%; Perigee, 96%; p = 0.62), mean ± SD patient satisfaction (Prolift, 8.2 ± 2.0; Perigee, 8.2 ± 1.8; p = 0.91), and complication rates did not differ significantly between the two groups.
Conclusions
The Anterior Prolift® was found to not differ significantly from Perigee® at 11 months.
Similar content being viewed by others
Abbreviations
- POP-Q:
-
Pelvic organ prolapse quantification
- RCT:
-
Randomized controlled trial
- POP:
-
Pelvic organ prolapse
- TVT-O:
-
Tension-free vaginal tape–obturator
- APFQ:
-
Australian pelvic floor questionnaire
- SD:
-
Standard deviation
- SUI:
-
Stress urinary incontinence
- UTI:
-
Urinary tract infection
- IDC:
-
Indwelling catheter
- CISC:
-
Clean intermittent self-catheterizations
- ADL:
-
Activities of daily living
References
Feiner B, Jelovsek JE, Maher C (2009) Efficacy and safety of transvaginal mesh kits in the treatment of prolapse of the vaginal apex: a systematic review. BJOG 116:15–24
Nguyen JN, Burchette RJ (2008) Outcome after anterior vaginal prolapse repair: a randomized controlled trial. Obstet Gynecol 111:891–898
Nieminen K, Hiltunen R, Heiskanen E, Takala T, Niemi K, Merikari M, Heinonen PK (2008) Symptom resolution and sexual function after anterior vaginal wall repair with or without polypropylene mesh. Int Urogynecol J Pelvic Floor Dysfunct 19:1611–1616
Sivaslioglu AA, Unlubilgin E, Dolen I (2008) A randomized comparison of polypropylene mesh surgery with site-specific surgery in the treatment of cystocoele. Int Urogynecol J Pelvic Floor Dysfunct 19:467–471
Maher C, Feiner B, Baessler K, Adams EJ, Hagen S, Glazener CM (2010) Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 4:CD004014
Altman D, Vayrynen T, Engh ME, Axelsen S, Falconer C (2011) Anterior colporrhaphy versus transvaginal mesh for pelvic-organ prolapse. N Engl J Med 364:1826–1836
Iglesia CB, Sokol AI, Sokol ER, Kudish BI, Gutman RE, Peterson JL, Shott S (2011) Vaginal mesh for prolapse: a randomized controlled trial. Obstet Gynecol 116:293–303
Maher CF, Feiner B, Decuyper EM, Nichlos CJ, Hickey KV, O'Rourke P (2011) Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial. Am J Obstet Gynecol 204(4):360.e1–360.e7
Fatton B, Amblard J, Debodinance P, Cosson M, Jacquetin B (2007) Transvaginal repair of genital prolapse: preliminary results of a new tension-free vaginal mesh (Prolift technique)–a case series multicentric study. Int Urogynecol J Pelvic Floor Dysfunct 18:743–752
Gauruder-Burmester A, Koutouzidou P, Rohne J, Gronewold M, Tunn R (2007) Follow-up after polypropylene mesh repair of anterior and posterior compartments in patients with recurrent prolapse. Int Urogynecol J Pelvic Floor Dysfunct 18:1059–1064
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO, Klarskov P, Shull BL, Smith AR (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Maher C, Dwyer P, Carey M, Gilmour D (1999) The Burch colposuspension for recurrent urinary stress incontinence following retropubic continence surgery. Br J Obstet Gynaecol 106:719–724
Baessler K, O'Neill SM, Maher CF, Battistutta D (2009) Australian pelvic floor questionnaire: a validated interviewer-administered pelvic floor questionnaire for routine clinic and research. Int Urogynecol J Pelvic Floor Dysfunct 20:149–158
Feiner B, Maher C (2010) Vaginal mesh contraction: definition, clinical presentation, and management. Obstet Gynecol 115:325–330
Long CY, Hsu CS, Jang MY, Liu CM, Chiang PH, Tsai EM (2011) Comparison of clinical outcome and urodynamic findings using “Perigee and/or Apogee” versus “Prolift anterior and/or posterior” system devices for the treatment of pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 22(2):233–239
Aungst MJ, Friedman EB, von Pechmann WS, Horbach NS, Welgoss JA (2009) De novo stress incontinence and pelvic muscle symptoms after transvaginal mesh repair. Am J Obstet Gynecol 201:73.e1–73.e7
de Tayrac R, Deffieux X, Gervaise A, Chauveaud-Lambling A, Fernandez H (2006) Long-term anatomical and functional assessment of trans-vaginal cystocele repair using a tension-free polypropylene mesh. Int Urogynecol J Pelvic Floor Dysfunct 17:483–488
Lowman JK, Jones LA, Woodman PJ, Hale DS (2008) Does the Prolift system cause dyspareunia? Am J Obstet Gynecol 199:707.e1–707.e6
Maher CF, Qatawneh AM, Dwyer PL, Carey MP, Cornish A, Schluter PJ (2004) Abdominal sacral colpopexy or vaginal sacrospinous colpopexy for vaginal vault prolapse: a prospective randomized study. Am J Obstet Gynecol 190:20–26
Nieminen K, Huhtala H, Heinonen PK (2003) Anatomic and functional assessment and risk factors of recurrent prolapse after vaginal sacrospinous fixation. Acta Obstet Gynecol Scand 82:471–478
Funding
The study was supported by a competitive research grant from the Australian Gynaecological Endoscopy Society (AGES), 2008, Sydney, Australia
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Feiner, B., O’Rourke, P. & Maher, C. A prospective comparison of two commercial mesh kits in the management of anterior vaginal prolapse. Int Urogynecol J 23, 279–283 (2012). https://doi.org/10.1007/s00192-011-1578-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-011-1578-x